August’s medical & legal story
Trouble downloading? Contact cgabbard@unf.edu
.
PART ONE: TO MAKE A LONG STORY SHORT…

Ilene pregnant at Baker Beach, San Francisco, 1999
In preparation for the birth of our first child, a boy we named August, my wife Ilene carried out all the measures expected of an enlightened mother-to-be living in a technocratic society. She and I undertook genetic testing before conceiving, looking for signs of Tay-Sachs, Cystic Fibrosis, and other conditions. Ilene underwent an amniocentesis early in the gestation period. She also followed the recommendations for a healthy pregnancy found in What To Expect When You’re Expecting and other sources. In the late winter and early spring of 1999, all test results pointed to healthy development.
Ilene’s pregnancy was deemed low risk, and her first doctor at the University of California, San Francisco (UCSF), the late Julian Parer, allowed the baby to go eleven days past the due date before inducing labor. And the two UCSF doctors managing the forty-three-hour labor, Sarah Kilpatrick (the attending physician whose specialty was perinatology and who is now practicing at Cedars-Sinai in Los Angeles) and Lisa Lipschitz (a resident at the time and now practicing at Scripps Health in San Diego), delivered the baby vaginally despite serious signs of distress coming from the fetal heart monitor at 2:55 a.m., forty-nine minutes prior to the birth at 3:44 a.m. Friday, March 5th.
Reading the monitor’s fetal-heart-rate (FHR) tracings at 2:55 a.m., the main labor and delivery nurse said, “These vitals are not reassuring. I don’t believe the baby’s heart rate should be this low.” Drs. Kilpatrick and Lipschitz dismissed the L & D nurse’s concern and the FHR tracings on the assumption that the monitor was either unreliable or malfunctioning.
Later, at the six-week postpartum check, Dr. Kilpatrick told Ilene that our son’s catastrophic birth was attributable to “bad luck.” And this was the only explanation that she or anyone at UCSF, for that matter, ever gave us. “Bad luck” was the official cause of our baby’s severe brain damage. All the data, evidently, pointed to this etiology.
In all likelihood, August’s delivery was a case of labor dystocia, obstructed labor, that went undetected. This at least is what an anesthesiologist who has taken part in many obstetric cases at Baptist Hospital in Jacksonville told us.
August’s official diagnoses were hypoxic ischemic encephalopathy, cerebral palsy, spastic quadriplegia, profound mental retardation, cortical visual impairment, microcephaly, seizure disorder, osteopenia, and more.
August Chazan-Gabbard died fourteen years later as a delayed outcome of the way he was delivered. And that’s the short version of his birth story.
.
PART TWO: THE LONG STORY

Ilene and I clowning around with diapered teddy bear before the birth, February of 1999
§
UNIVERSITY OF CALIFORNIA, SAN FRANCISCO (UCSF)

University of California, San Francisco
The choice of the hospital for the birth came down to two. California Pacific Medical Center, known locally as CPMC, a facility blocks from our apartment in the inner Richmond District, served the local community. Annually it performed three times more deliveries than did the University of California, San Francisco (UCSF) Medical Center.
Ilene was employed as a clinical professor of physical therapy at UCSF. Because it was her place of work and because she trusted the institution, she chose to have the birth there. Given that UCSF was one of the world’s leading hospitals, she had taken for granted that no problem should arise regarding the simple matter of delivering a baby.
As a clinical professor of physical therapy, Ilene had successfully treated the dean of the medical school (he had a problem with his knee), so, as a little ‘thank you,’ she was assigned one of the medical center’s V.I.P. delivery suites. Located at the Parnassus campus, it was the kind of birth suite reserved for the wives of rich oil sheikhs flown in from Saudi Arabia. It offered a panoramic view of downtown San Francisco.
Our friend Pattye Tobase, also a clinical professor of physical therapy at UCSF, first joined us in the V.I.P. birth suite about midday on Wednesday, March 3rd, 1999. Eight years younger than Ilene, she had short black hair, obsidian eyes, and a mischievous grin. She was frequently with us during the labor and present at the delivery.
§
UCSF DOCTORS INVOLVED WITH THE BIRTH

Dr. Sarah Kilpatrick, now at Cedars Sinai Medical Center in Los Angeles
August was delivered by Dr. Sarah Kilpatrick. UCSF being a teaching hospital, she served as the attending physician. She is a perinatologist, a doctor trained in the subspecialty of obstetrics concerned with the care of the fetus and high-risk or complicated pregnancies. Such a doctor is supposed to be highly skilled in prenatal diagnosis. According to the website of the Cedars Sinai Medical Center, where she is currently the chair of its Department of Obstetrics and Gynecology, she “is a nationally renowned expert in maternal-fetal medicine and women’s health.” She is also a prolific producer of scholarly research articles.

Dr. Lisa Lipschitz, now at Scripps Health in San Diego
The resident physician (a doctor in training) under Dr. Kilpatrick’s supervision was Dr. Lisa Lipschitz. She now practices medicine at Scripps Health in San Diego.

Dr. Julian Parer, deceased
A third doctor, Dr. Julian Parer, was the attending physician on Wednesday, March 3rd, when Ilene first arrived at the hospital. He was a doctor with a marvelous bedside manner. Years later, in 2016, we were sad to learn that he died while hiking in the hills of the Bay Area. Coincidentally, he had written a textbook on the subject of how to interpret fetal-heart-monitor readings.
§
DUE DATE: FEBRUARY 20th, 1999
The baby’s due date arrived, February 20, 1999, a Saturday. By Monday, the baby had not come, but the medical staff with whom Ilene interacted never deemed her pregnancy to be high-risk, so we weren’t worried. To pass the time, we attended a matinee screening of Terrence Malick’s war movie The Thin Red Line at a theater in the Marina District. During the closing credits, Ilene sensed for the first time that the baby was not as active as it had been. In fact, she felt no fetal activity at all and suspected that something was wrong.
After the movie she went to the office of her OB-GYN at UCSF, the Parnassus campus, where the fetus underwent tests. Her OB-GYN was part of an all-woman practice. The nurse said the results didn’t look good: the numbers were low and very worrisome. She told Ilene to go up to the fifteenth floor of UCSF, also at the Parnassus campus. There a young male resident physician repeated the tests, carrying them out hurriedly. Ilene told me afterward that he seemed extremely tired.
“Your baby is fine,” he said, somewhat dismissively, when he was finished.
On Monday, March 1st, ten days after Ilene’s due date, the test results again were “not good.” The numbers were troubling. Yet the nurse conducting the tests said reassuringly, “Your baby is fine.”
“Are you certain?” said Ilene.
“Absolutely.”
“I think there’s something wrong.”
“Come back in two days and Dr. Parer will oversee your induction unless you go into labor before then. All expectant moms worry too much. Everything will be all right. Come back in two days. We’ll get that baby out.”
§
DOCTOR DASH SMOKE
We arrived at UCSF’s Parnassus campus hospital before 9 a.m. on Wednesday morning, March 3rd, for Ilene’s induction to begin. Dr. Parer was the attending physician, but, just hours later, at about midday, he rotated off and was replaced by Dr. Kilpatrick. Dr. Lipschitz, the resident physician, also came on duty.
The resident was the physician managing the birth because Dr. Kilpatrick was rarely in the delivery suite. Due to Dr. Kilpatrick’s habit of dashing into the room only to immediately dash out again, seemingly leaving a trail of smoke in her wake, Ilene, Pattye, and I humorously dubbed her “Doctor Dash Smoke.”

Ilene had hoped to forego pain-relief but found she couldn’t, so later that same day, Wednesday, at about 2 or 3 p.m., an anesthesiologist gave her an epidural.
About 7 a.m. Thursday, a new nurse, a black woman in her mid-thirties, became our primary Labor and Delivery (L & D) nurse.

Ilene, Thursday morning, March 4, 1999
A little past midday on Thursday, a severe pressure pain developed in Ilene’s lower pelvis. This pain was pushing through the numbing effects of the epidural.

Ilene, Thursday, March 4
“I’m sure something is wrong,” said Ilene to the resident on Thursday afternoon. “It feels as if the baby’s stuck, like it’s impacted against my pelvic bone.”
“Everything is going well,” replied the resident. “That baby will be out in no time.”
Ilene insisted: “It feels like things are jammed up in there.”
The resident again reassured her.
But, despite the epidural, the pain in her pelvic region continued to intensify, and she developed a fever. During this period, we had seen Dr. Dash Smoke for only fleeting moments.
Late Thursday afternoon, the L & D nurse and a second nurse got Ilene out of bed in order for her to walk and progress the labor, which had stalled. Tethered like an astronaut to monitors on a rolling IV pole, Ilene managed to take a few steps with Pattye’s and my assistance, but then the L & D nurse approached in a panic and hurried her back into bed. The electronic fetal monitor (EFM) indicated that the baby’s heart rate was dropping.
Once settled in bed, Ilene was reassured by the L & D nurse that everything was fine. She turned to the EFM, which was methodically churning out a stream of narrow paper like a 1928 ticker tape, gathered up a stretch of it, and held it up.
“This is where the baby’s heart rate went down,” she said, pointing with her index finger, “and this is where the heart rate came back up.”
§
THE FETAL HEART MONITOR: 2:55 A.M.
Nearly two days after we arrived at the hospital, in the post-midnight hours of March 5th, Ilene was in her fortieth, forty-first, and forty-second hours of labor.
Around 2:10 a.m., Pattye left the birth suite briefly to retrieve something from her apartment, which was several blocks down the hill from the Parnassus campus on Hugo Street between Fourth and Fifth Avenues. At approximately 2:55 a.m., the primary L & D nurse noticed that a problem was showing up on the fetal-heart monitor and said to a second nurse, “The baby’s heart rate is low.” The two discussed whether the monitor was picking up the mother’s heartbeat or that of the fetus. The resident joined in this quiet discussion and speculated that a problem was occurring with the monitor, not the baby.
“Must be mom’s,” the resident said of the fetal heart rate. She followed up by telling the two nurses something to the effect that fetal-heart monitors were not always reliable. She then stepped out the door for about thirty seconds. The L & D nurse wasn’t convinced. She seemed perplexed and asked the other nurse again if the reading could have been the baby’s. The other nurse didn’t answer. The L & D nurse then said, “These vitals are not reassuring. I don’t believe the baby’s heart rate should be this low. It’s in the eighties.”
“Must be mom’s,” the other nurse replied, repeating what the resident had said. Her tone was matter of fact.
“That doesn’t seem right,” responded the L & D nurse, her intonation more urgent.
The L & D nurse was conveying that the fetus was experiencing stress, the eighties being below the acceptable range. A normal range for a fetus runs between 110 and 160 heartbeats per minute. This is much faster than the mother’s heart rate. I have been informed that a pulse of 80 beats per minute in a laboring mother is on the low end of typicality.
What the L & D nurse was trying to tell the resident physician and then the other nurse was that she was detecting signs of bradycardia. Bradycardia signals that the baby is in distress and that the delivery team will have thirty minutes to get the baby out, usually by C-section.
The L & D nurse was relying for this information on an EFM. According to the Health Encyclopedia page of the University of Rochester Medical Center, “[f]etal heart rate monitoring is a procedure used to evaluate the well-being of the fetus by assessing the rate and rhythm of the fetal heartbeat. During late pregnancy and labor, [a] physician may recommend monitoring the fetal heart rate and other functions. The average fetal heart rate is between 110 and 160 beats per minute, and can vary five to 25 beats per minute. The fetal heart rate may change as the fetus responds to conditions in the uterus. An abnormal fetal heart rate or pattern may indicate that the fetus is not getting enough oxygen or that there are other problems.”
The U of Rochester Medical Center page goes on to say, “Internal fetal heart rate monitoring uses an electronic transducer connected directly to the fetal skin. A wire electrode is attached to the fetal scalp or other body part through the cervical opening and is connected to the monitor. This type of electrode is sometimes called a spiral or scalp electrode. Internal monitoring provides a more accurate and consistent transmission of the fetal heart rate than external monitoring because factors such as movement do not affect it. Internal monitoring may be used when external monitoring of the fetal heart rate is inadequate, or closer surveillance is needed.”
The resident stepped back into the birth suite and, when questioned again by the L & D nurse, reiterated that the heart rate must be the mother’s. The resident considered it a nonissue, and the L & D nurse dropped the matter.
Dr. Kilpatrick was not present during the exchange about the monitor that took place among the resident, the L & D nurse, and the second nurse, with me eavesdropping.
In retrospect, by which I mean from an historical perspective, the question to consider is, if the reading had been of the mother’s heart, wouldn’t that have meant that the baby’s heart was going unmonitored? To the best of my recollection, the resident did not check Ilene’s pulse rate by taking a pulse, looking at an EKG, or using a pulse oximeter and comparing what any of these was reporting to what the EFM was indicating.
Even if the resident took one of these actions though and I missed it, I never heard her and/or the nurses talk about following up by repositioning the scalp electrode (the EFM’s sensor on the fetus) so that the monitor was ascertaining the baby’s heart rate. And even if I missed that too, I never heard anyone say words to the effect of, “Oh, THERE’S the baby’s heart beat!”
The telemetry associated with the EFM had gone awry. The premise of EFM was to communicate to medical personnel outside the womb the health status of the fetus inside the womb, and if there was a technical problem, it needed to be corrected. Otherwise, why bother to use the technology!
In August’s case, no one seemed to be relying all that much on a monitor. I can only infer that both Dr. Kilpatrick and Dr. Lipschitz were skeptical of it. I say this judging from their words and body language: they appeared to assume that it just wasn’t all that useful or that it must have been malfunctioning. At 2:55 the resident had told the nurses that monitors were not always reliable. And at 3:33 a.m., Dr. Kilpatrick would ask the resident “There was a problem with the monitor?”
Years later, after August died in 2013, I went online to read up on EFM and found the guidelines of the American Congress of Obstetricians and Gynecologists, which state, “When EFM is used during labor, the nurse or physicians should review it frequently.” I also looked for an article roughly contemporaneous with the time of August’s birth to find out what Kilpatrick and Litpschitz might have been thinking. Was there some opinion circulating at the time that EFM wasn’t reliable? I found a May 1999 article in American Family Physician examining the limitations of EFM, which evidently are numerous. It reported that some clinicians believe that EFM provides valuable information but that it takes an expert to properly interpret the results. This was where August didn’t benefit from the luck of the draw because, as I said earlier, Dr. Parer, the attending physician on duty when Ilene and I came in on Wednesday morning, March 3rd, was an authority on interpreting EFM results.
By the way, EFM produces a chronological record of the birth both digitally and in paper form. As I mentioned earlier, these little machines spin out a continuous thin paper strip, also called “tracings,” that provides a read-out of a fetal heart rate. The tracings literally become the birth’s paper trail.
In any case, the EFM’s internal sensor on the fetus would be removed around 3:10 a.m., thirty-four minutes prior to the birth.
§
DESERTED IN THE V.I.P. DELIVERY SUITE: 3:15 to 3:27 A.M.
Pattye returned to the delivery suite shortly after 3 a.m. At approximately 3:03 a.m., Dr. Kilpatrick stepped in for less than a minute. The resident told her that a problem was occurring with the heart monitor. Kilpatrick didn’t respond, and the resident didn’t repeat herself. Kilpatrick obviously was in a hurry. Before dashing out, however, she unexpectedly shouted, “We’re going to have a baby!” This exclamation seemed so out of character that I did a double take. Then she was gone.
Shortly after Dr. Kilpatrick’s departure, Ilene was found to be maximally dilated. Dr. Lipschitz, the L & D nurse, and another nurse set up a sterile area and adjusted the bed from a sleeping to a delivery arrangement. They positioned Ilene on her back with her hips and knees maximally flexed. As I said earlier, at 3:10 a.m. the fetal heart monitor attachment was removed. These preparations concluded, a long pause ensued. Then, Dr. Lipschitz and the second nurse scattered to the hallway, leaving just Ilene, Pattye, the L & D nurse, and me.
By 3:15 a.m. the room had grown eerily quiet. Then the L & D nurse said, “I’m going to check on something,” and she scurried off too, leaving Ilene, Pattye, and me by ourselves.
The three of us were left completely alone in the birth suite from approximately 3:15 to 3:27 a.m.
More minutes went by. The three of us began to feel like passengers on a ship that has been abandoned by its crew. Pattye asked, “Where the hell did everybody go?”
I shrugged. I had no idea what was going on.
“I wonder if the nurses and Dr. Lipshitz are trying to round up the pediatric team,” speculated Pattye, and then she said, “Cowboy! Go see what’s happening!”
Her suggestion made sense. Go find help! As I was exiting I said, “Where should I go?”
“The nurses’ station!”
I exited the suite and jogged to the nurses’ station down the corridor. The clock on the wall there said 3:23 a.m.
“My wife’s ready to give birth,” I said meekly. “Where are the doctors?”
Behind the desk, a middle-aged blond nurse was standing and gazing at a computer screen. She replied, “Everyone’s giving birth. They’ll come when they can.”
“Will the doctors be coming soon?”
“They’re very busy.”
“Oh, I’m sure they are,” I said, apologetically. “I wouldn’t want to trouble them. But I just want them to know that my wife is ready.”
“Ready?”
“To give birth,” I said, clarifying.
She looked at me quizzically. “It depends on what you mean by ready.” Deciding not to debate the matter further, she continued, “I’ll let them know. They’ll be along. Don’t worry.”
Since she didn’t ask me which doctors were ours or even who I was, I continued: “Dr. Kilpatrick is the attending physician. Dr. Lipschitz is the resident. I’m Gabbard. My wife is Chazan. We’re in suite 1524.”
She looked up again. “They’ll come when they can.” Then, giving me an encouraging wink before returning to her screen, she added “They’ll get that baby out in no time.”
The fact that the hospital was overwhelmed with so many mothers giving birth at the same time indicated that it was short staffed. Not having enough personnel on hand explained why our own main L & D nurse was also a per diem nurse who had been called in from Sacramento.
I left the nurses’ station and began looking for someone, anyone, to draw attention to our situation. Really wanting to find a doctor, I wandered the gleaming corridors of what seemed like a high-end spaceship, like the one Octavia Butler describes in Dawn. The place was empty, yet the walls hummed with life. Through an invisible mesh of faint voices and muffled sounds I made my way. I was specifically looking for Dr. Kilpatrick, Dr. Lipschitz, the L & D nurse, and the second nurse, but I didn’t find any of them. At 3:25 a.m., I stepped back into the suite, but still, the only ones occupying the room were Pattye and Ilene.
“You lie!” Pattye exclaimed when I repeated what the nurse had said to me.
“The nurse at the desk seemed to think this is going to be a very easy birth,” I said.
“I’m going down to the nurses’ station myself and make a big stink,” said Pattye, and she was just about to stomp down there and complain loudly when the L & D nurse and the other nurse returned. That was at 3:27 a.m. Shortly after, Dr. Lipschitz followed them in. She seemed remarkably composed.
§
A RELAXED ATMOSPHERE:
3:28 TO 3:41 A.M.
From the time Dr. Lipschitz re-entered the suit at approximately 3:28 a.m., she, the L & D nurse, and the second nurse appeared to be waiting for something to happen.
At 3:33 a.m., Dr. Kilpatrick came into the birth suite. She obviously heard what Lipschitz had said to her at 3:03 a.m. because the first thing she asked when she reappeared was, “There was a problem with the monitor?” A short and seemingly casual conversation followed with Dr. Lipschitz about whose heart rate the now-detached fetal monitor had been reading at 2:55 a.m. Given the low numbers, Dr. Kilpatrick quickly affirmed, “Yes, it must have been the mother’s.” The two doctors were completely at ease, exhibiting no sense of urgency. Dr. Kilpatrick took her time as she gowned and gloved up. I remember being impatient with her slowness.
Later, in her legal deposition, Dr. Kilpatrick declared under oath that it was at 3:33 a.m. that she first became aware of a problem in the delivery suite.
Shortly after she came in, a specially dispatched pediatric team of seven or eight residents and medical students suddenly roared through the door. Why they were there or who summoned them I have no idea. This was at about 3:35 a.m. They wheeled with them a small table and used it to establish a makeshift station ten feet to the left of the end of Ilene’s bed.
The residents and medical students were full of good cheer. The only female among them was a tall, young, and slender Asian woman with a long black ponytail. She was a senior resident physician, and she was more serious in bearing than the other team members. Later that day she came to speak with us, to express her concern. She was the only one of all the medical professionals present in the delivery suite that morning who did.
§
THE BIRTH:
3:42-3:50 A.M.
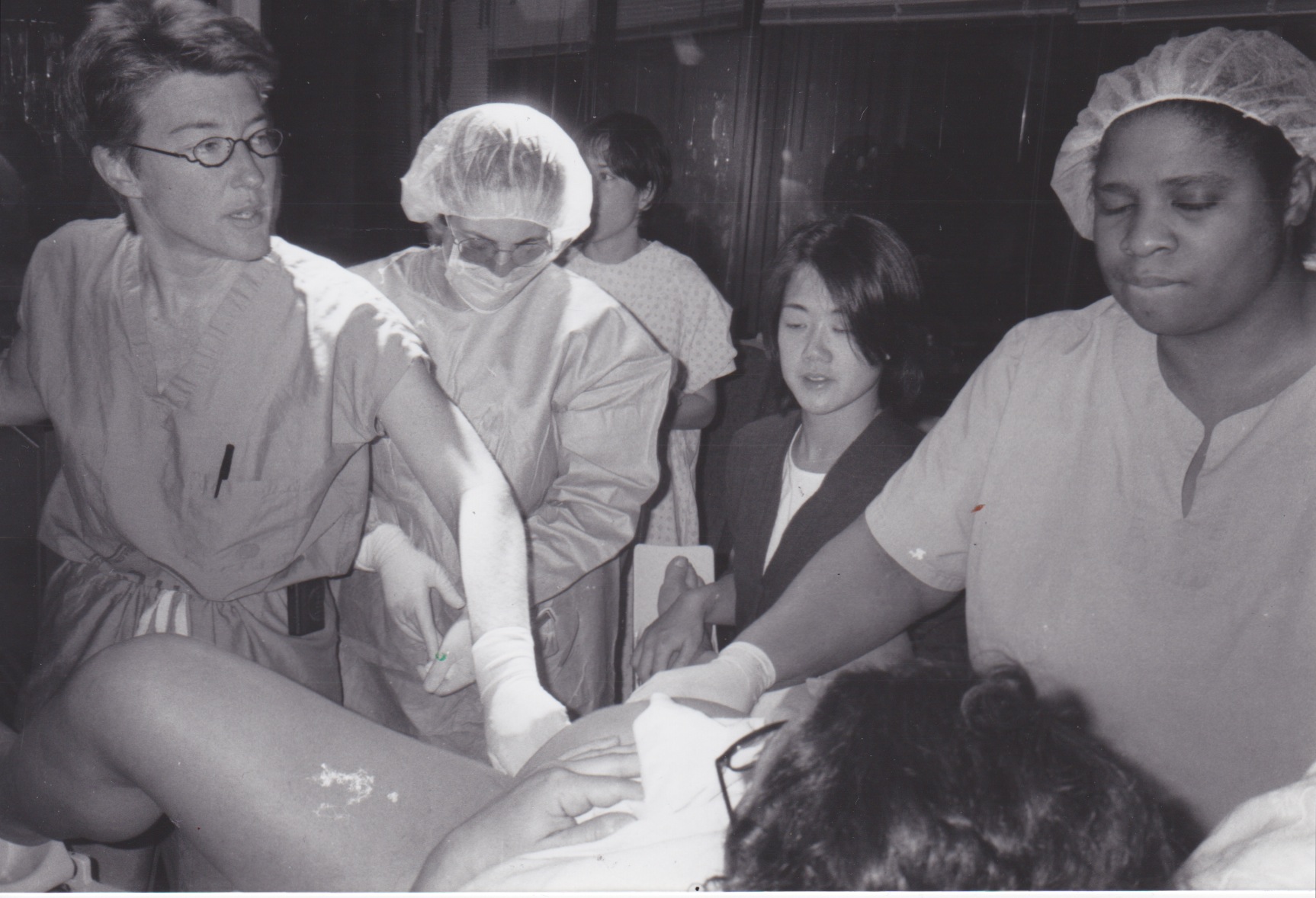
Moments before August’s birth. Dr. Sarah Kilpatrick on the left, Dr. Lisa Lipschitz, Pattye Tobase, and the primary labor-and-delivery nurse.
The baby’s head began to crown (or was crowning) at around 3:41 a.m. This is the time when Dr. Kilpatrick went down on one knee between Ilene’s spread legs. It must have been about 3:42 a.m. that I saw her eyes pop wide open. Instantly the expression on her face became one of extreme concern, a countenance that was quite different from the relatively neutral one of a moment before. Her attention suddenly became tightly focused, like that of a pilot when a plane suddenly shows signs of trouble in flight. She called to the nearby team, “There’s an abrasion on the baby’s head!” And then, almost immediately after, she shouted, “We’re going to use the vacuum!”
Dr. Lipschitz and the D & L nurse sprang into action and swiftly readied the gear. Standing again, Kilpatrick positioned the vacuum-extraction device and told Ilene to push, and she obeyed, and then came another order to push, and on the third try there was a great whoosh, liquid gushing, and with a flood of brownish amniotic fluid, the infant tumbled out headfirst.
At 3:44 a.m., the baby emerged gray, limp, and lifeless. His color was appalling: grayish-green, like that of a stillborn baby.
The fetal heart monitor evidently had been working correctly all along.
The umbilical cord was wrapped twice around the baby’s neck. Dr. Kilpatrick hurriedly clamped and cut the cord and handed the newborn to the resident behind her, who whisked him over to the specially dispatched team where the residents were waiting. The team began attempting to resuscitate him.
Everyone’s activity seemed frantic, and everyone whose faces we could see had wide-open eyes and grim “Oh no!” expressions. Everyone’s, that is, except for that of Dr. Kilpatrick, who had never really lost her composure except for that brief moment at 3:42 a.m. when she seemed to first discover that there was a problem. During these tense moments she acted as though nothing were amiss. All the while, the baby didn’t cry. He didn’t make any sound at all. For the first minute, most of what Ilene, Pattye, and I could see was the scrum of residents’ and students’ backs.
Dr. Kilpatrick was standing near Ilene’s delivery bed, and she reassuringly informed us: “The baby is merely stunned.” Contradicting this verbal assertion though were the apprehensive looks of others, whose faces were becoming more and more visible. Some of them had begun peeking at us, as though to see what our reaction was. The tall Asian female with the ponytail and I exchanged a mutual gaze, and I knew then from her horrified expression that things were going very badly.
I wasn’t looking at Pattye, but I heard her mumble, “I can’t believe this is happening.”
The L & D nurse walked toward Ilene’s bed, moving so slowly that she seemed to advance frame by frame, as if all of this was the footage of a dream. As she approached, she held my gaze as though communicating something important. I didn’t know then, but I know now what she was silently communicating. As with almost everyone else, her eyes were wide open and worried.
The notable exception was Dr. Kilpatrick, who spoke again, as calmly as before, saying, “This sort of thing happens all the time.”
We were all waiting for the baby to breathe. But how many minutes were going by? When he finally began breathing, everyone exhaled. It was cause for celebration. Still, the newborn wasn’t crying or making a sound loud enough to hear. I could tell from her demeanor that tall resident with the ponytail was convinced that a calamity was still unfolding. Not so the others. A little party had broken out: the residents were cheering and the students started high fiving. She quickly shushed them. She was the only one who seemed to realize that, by the time August started breathing, the brain damage had already been done.
“Show Mom and Dad the baby!” called Dr. Kilpatrick optimistically. She was still standing beside Ilene’s bed. A male resident next to the female resident complied, and he hoisted the little body high into the air, a trophy of medical rescue. The baby’s color was still grayish-green, like that of a stillborn baby. His eyes were shut, he wasn’t making any sounds, and he wasn’t moving at all, as though he were non-responsive. The resident very well could have been holding up the body of a dead baby.
§
FIFTY-FIFTY CHANCE OF SURVIVAL
The newborn was whisked away to the Intensive Care Nursery (ICN) in the Benioff Children’s Hospital, which was housed in the same building.
Now 4 a.m., the V.I.P. delivery suite was again quiet. Dr. Kilpatrick was gone. The birth had occurred less than fifteen minutes earlier, but already she had left. Other babies needed to be delivered. The hospital had rarely experienced such a high volume of births all at one time, so she’d had to race off to the next one, taking our L & D nurse with her. Dr. Lipschitz, a second nurse, and a third nurse we’d not seen much were performing the aftercare on Ilene.
We had to vacate right away. Pattye wordlessly helped me gather our things. She looked like a person dazed in the wake of a car wreck. As soon as we got the signal that the resident and the nurses were finished, Pattye broke the silence, saying in a small voice, “We’re done here.”
The recovery room was the opposite of what the labor and delivery suite had been. The luxury accommodation gave way to a dark, cramped cubicle. At this point, Pattye silently hugged us and headed home.
Within forty-five minutes, Ilene and I heard a gentle knock. Two male physicians entering, they began with the only good news there was: no meconium (the first feces of a newborn infant sometimes released in utero moments prior to the birth) had been found below the infant’s vocal cords. And then came the rest. Physicians use a method called Apgar, based on a 1–10 scale, to quickly summarize the health of a newborn, and an infant with a score of 8 or above is considered to be in good shape. Our newborn’s Apgar scores were 2, 3, and 4 in the first ten minutes—abysmal.
“The infant has lost a lot of blood,” said the first doctor, “and so will need a transfusion, preferably with blood provided by one of the parents.”
“Can you donate?” asked the second, finishing the other’s thought and directing the question to me.
“Seizure activity has been noted,” the first doctor added. He asked us to sign a consent form for a lumbar puncture. This puncture, I found out later, would be just the first of three.
“The newborn’s condition is critical,” the second doctor said. He didn’t mince words. “The chances of survival are fifty-fifty.”
“You can go up to the ICN,” said the first doctor in a lowered tone intended for me, “but your wife should remain in bed to recuperate.”
§
IN THE ICN:
BENIOFF CHILDREN’S HOSPITAL
MARCH 5th–15th
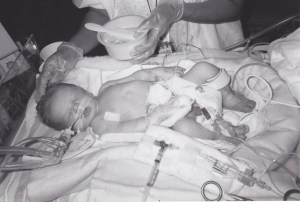
August spent ten days in the intensive-care nursery or ICN (UCSF Benioff Children’s Hospital)
I went up to the ICN at about 6 a.m. of March 5. Critical-care personnel bustled urgently on the far side of his isolette. Our baby lay within, utterly still. Heavily sedated, he of course was not awake. He was lying on his back with his knees bent, fists clenched, toes curled, and eyes closed, and he was breathing with the aid of a ventilator.
Save for the tiniest of diapers, his flesh was fully exposed. The earlier greenish-gray stillborn color he’d been born with had pinked up somewhat. Above the body, an extremely bright light radiated warmth. Electrodes covered his body, and a jungle of wires and lines relayed back and forth between the tiny form and several monitors and machines. An apparatus would occasionally sound an alarm, and someone would rush over to see what was happening.
His head was of seemingly typical size and shape for an infant but with a large laceration. It was a deep red impression on the forehead. The head must have been pressed firmly for a long time against some hard internal impediment. This might have had something to do with the pain Ilene had been feeling in her back during much of the labor, the pain the epidural couldn’t alleviate. Why was it there? It was a mystery.
The next day, Saturday, Ilene and I were told that August had been enrolled in a BAMRI (birth asphyxia MRI) study. As a baby born with a brain injury, he had undergone an MRI, and the team associated with the study would conduct follow-up examinations in the months and years to follow. This team would eventually be instrumental in developing the CritiCool control unit, a device that reduces brain swelling in asphyxiated infants via a cooling cap. These would come online roughly ten years after August’s birth and become standard protocol. In other words, August was born a decade too early to take advantage of this breakthrough, but, in a small way, he contributed to making it possible.
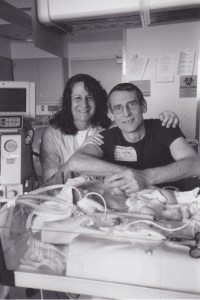
Mom and dad with August in the ICN
On Monday, March 8, August opened his eyes, which at the time were unequivocally green. Then, like the waters of a hundred-year flood, the lines, catheters, wires, and tubes over the subsequent days began receding from his body.

August’s uncle Jesse and aunt Cristina pay August a visit in the ICN
On Wednesday, a repeat EEG failed to capture more seizure activity, but it “did show flattened baseline.” By then Ilene and I had begun to hold and bathe the baby and change his diaper. By turns he was floppy and rigid. On Thursday Ilene spotted on a table next to August’s isolette a nurse’s index card. On it were scrawled the phrases “serious neurologic dysfunction” and “poor prognosis.”
Eventually August stabilized, and the question changed from whether he would live to what his quality of life would be.
§
FAMILY CONSULTATION:
MARCH 12th
The hospital scheduled August for discharge on Monday, March 15, but before it could release him its representatives had to sit down with us. On the preceding Friday, March 12, at 11 a.m., we all assembled in a windowless conference room somewhere in the bowels of the enormous institution. This was the “family consultation” or “family consult,” one of a myriad of undertakings that the national accrediting organization— the JCAHO (formerly known as the Joint Commission on Accreditation of Healthcare Organizations, now simply the Joint Commission)—required of UCSF. In situations like ours, the JCAHO compelled the hospital to supply representatives to meet with the family.
Green as an Oregon forest, I’d had high expectations going in to the family consult. The doctors would solve the riddle of what happened to our son? My idealistic expectations were speedily dashed. The hospital representatives were not going to reveal any information that might provide grounds for litigation.
Dr. Kilpatrick and Dr. Lipschitz did not attend. And no one from the all-female OB-GYN practice with which Ilene had undertaken her prenatal care was there either. We wanted desperately to speak with them, but we were told that their busy schedules precluded them from being present.
Instead, we met with five other hospital representatives, four male doctors, all wearing white lab coats, and a lone woman, a social worker. Two of the doctors we somewhat knew: we had seen the senior resident physician and the neurologist in the ICN. Ilene and I sat on one side of a long conference table, and the four physicians sat on the other. The social worker sat behind them.
We were told that August suffered from hypoxic ischemic encephalopathy or H.I.E. This was caused by a lack of blood and oxygen due to events unknown occurring prior to or during his delivery, bringing about very severe brain damage. Other diagnoses and labels for chronic and disabling conditions stemmed from H.I.E. They were cerebral palsy, spastic quadriplegia, profound mental retardation, cortical visual impairment, microcephaly, seizure disorder, osteopenia, and so forth.
We asked them why a pregnancy that had gone so well had concluded in such a horrific way? And we asked them how an experienced practitioner like Dr. Kilpatrick could have failed to detect a major problem in the delivery room? Ilene and I found ourselves in a dance with the four doctors in which each of them found creative ways to not answer our questions. They would not explain what happened. They would not account for what had gone wrong. They would not say anything beyond describing the baby’s current condition. They were not interested in solving the riddle.
The social worker said, “Getting him started with physical and occupational therapy is crucial. I will get you a referral for the Golden Gate Regional Center’s Early Intervention Program.” Because of the baby’s extremely serious condition, she went on to say, he would qualify straightaway for the Medi-Cal waiver, known in other states as the Medicaid waiver.
On some invisible signal, the meeting started winding down. One of the doctors leaned back and cradled his neck with his hands so that his elbows fanned up like wings. Looking like a bird in flight, he asked, “What are your plans?”
“Our plans?” This was a strange question. For a moment I thought about the future. It seemed like we didn’t have one. I felt like a man on a scaffold with the noose around his neck and the executioner asking, “What are your plans?”
At last I answered, “We plan to learn how to give our baby phenobarbital.”
As if simultaneously hearing the same cue, they all rose. The meeting was over. It had lasted forty-five minutes.
Ilene and I never saw or heard from these five individuals again, save for social worker, who secured the referral she had promised. Otherwise, this meeting was the last official contact we would have with UCSF regarding the birth, with two exceptions. One was the hospital’s patient satisfaction survey.
The other was Ilene’s postnatal visit with Dr. Kilpatrick roughly five weeks later. The most information she offered Ilene at the postpartum check about August’s birth was that it was “bad luck.” As a woman of science, Ilene didn’t find this explanation satisfying.
§
HUMPTY DUMPTY

Sophia Lowrie, August’s cousin

Reuben Case-Gabbard, Sophia’s brother and August’s cousin

Ilene and August on Baker Beach, San Francisco, 1999

August, early months
Six months after August’s birth, in the first week of September, the BAMRI study people showed up at our apartment on 21st Avenue in the Richmond district and had no sooner begun their tests with August than they began packing up their tools. They didn’t say why, but I knew why.

August, 1st year
§
1999-2013:
LAZARUS IN A WHEELCHAIR
Pulled back from the brink of death, August became Lazarus in a wheelchair. During his fourteen years, he was nonverbal, incontinent, spastically paralyzed, and cortically blind. He could not sit in a chair the way a typically developing child would. He needed upper trunk support, so he had to be secured in his wheelchair with straps holding his shoulders and chest in place. Propped upright, his head lolled, falling forward and backward: the muscles in his neck never developed properly. He also drooled, and this occurred because the spasticity affecting his mouth prevented him from being able to swallow his saliva efficiently. When he was lying on the floor, he was unable to crawl, scoot around, hold himself up, roll over, or even touch his toes. If someone were to put him in one spot and leave him there, he would be found in the same location an hour later, give or take a few inches.

Despite his rough start, August was a blithe spirit. I don’t know how to account for his happiness except to attribute it to the indomitable exuberance of youth. In all, he was a very nice person, and we had a wonderful father-son relationship. Some people have asked me, “would you have chosen your child knowing in advance that he would be so impaired?” I respond that no parent ever winds up with the child they imagined at the beginning they would have. Something said by Dhipthi Brundage, a psychiatrist in Durham, North Carolina, strikes me as true: “every good parent CHOOSES their child again and again. That’s all that matters.”
§
LEGAL CASE (1999-2004)
One of the take-away lessons Ilene and I learned from our experience of birthing a child at UCSF was this: if a hospital makes a mistake during a birth, and the child will require a lifetime of care on account of it, costing hundreds of thousands if not millions of dollars, no one from the institution runs after the parents as they are exiting the doors with their new baby to hand them a check.
Over the next five years and heading into the early aughts, I learned a valuable lesson–that it’s a heck of a lot harder to sue for medical malpractice than people think it is.
In the beginning August was so small, just a peanut, our “little bug,” and so it was hard for us to imagine that he wouldn’t always remain easy to care for. But we weren’t facing facts. We didn’t want to sue the hospital because we believed that only greedy, litigious people did that sort of thing. Having grown up in a family earning its living through a small business, I inherited the prejudices of that class, one of which is a deep-seated animosity toward lawyers.
However, my dissertation advisor at Stanford, John Bender, told me to seek counsel. And he was far from alone. A Bay Area group, Support for Families of Children with Disabilities, assigned Ilene to a mentor, Betty Lituanio, and Betty laid it on the line in the strongest possible terms, recommending to Ilene that we needed to take legal action now, not for ourselves but for August. He would require a great deal of financial support just to survive. The cost of his care over his lifetime, depending on how long he lived, easily could run into the millions of dollars. We needed to litigate on his behalf. He was the plaintiff, not us. If our son had been treated wrongly, it was his parents’ duty to seek justice.
Friends and family members began advising us that we were heading into an extremely rough future. The expense of caring for August down the line would become exorbitant. There would be the need for medications, therapies, treatments, surgeries, wheelchair-accessible vans, and around-the-clock attendants. There would be the need for adaptive equipment such as a hospital bed for the home, a lift, and pricey assistive devices. There would be the need for home modifications such as the widening of doors and installing wheelchair ramps, both outside and inside the house. There would be the need to reconstruct a shower to accommodate a wheelchair user and the caregiver bathing him. There would be the need for a lifetime supply of diapers. Right now, they warned, he was small, cuddly, and relatively manageable. But in time he would grow, and his needs would overwhelm us.
When we eventually decided to bring a case, our main objective was to solve the riddle of what happened to our son? But over time we discovered that suing to solve a riddle was naive because solving a riddle was not going to pay an attorney’s bills. It as a matter of pure economics: the cost of litigating a case and winning it in court can cost an attorney tens of thousands, sometimes hundreds of thousands of dollars.

Chris, Ilene, and August at the Beach Chalet, San Francisco, 1999
Ilene and I believed that the doctors had been negligent in three areas during the delivery process, each item more serious than the previous. First, they had not taken the worrisome test results of February 22 and March 1st seriously, delaying induction until March 3rd, many days after the due date. Second, they had ignored Ilene’s complaints during the labor about pain in her pelvic area. And third, the resident ignored the L & D nurse’s warning at 2:55 a.m. about the baby’s low heartbeat. We were confident that August’s birth records, which included the EFM’s tracings, would reveal the truth of the matter.
§
THE MEDICAL INJURY COMPENSATION REFORM ACT OF 1975 (M.I.C.R.A.)
Between mid-1999 and mid 2001, Ilene and I worked with two lawyers to pursue August’s birth injury case. The first, Allan Lerch, whom we referred to as “the pit bull,” we thought too aggressive, so we fired him. The more fools we to have ever thought anything could go wrong with being too aggressive when it came to battling UCSF. The second, Kevin Domecus, spent about a year deciding whether to take our case.

August in duck outfit, 2000
During this year we were waiting to hear, we learned that California was a “capped” state. California’s Medical Injury Compensation Reform Act of 1975, signed by Jerry Brown the first time he was governor and also known as M.I.C.R.A., placed a cap on pain-and-suffering damage awards. The cap, $250,000, may have been reasonable in 1975, but the cap had not been, and still–in 2021–has never been adjusted for inflation. I am going to repeat myself so there’s no misunderstanding: the $250,000 cap the state legislature imposed in 1975 remains the same in 2021. It’s the same now as it was forty-six years ago. An inflation calculator indicates that $250,000 in 1975 is the equivalent today of $1,254,692.
The cap has never been adjusted for inflation due to the power that the doctors’ lobby wields in the supposedly “progressive” California state legislature. Accordingly, it is virtually impossible these days in that state for a medically injured patient to have their day in court, much less win a medical malpractice suit. Considering that reputable sources believe that medical error is the third leading cause of death in the United States, this lack of access to the courts should be concerning for everyone.
Domecus finally turned down our case, and it was painfully obvious by then that M.I.C.R.A. was the reason why. In 2001, a cost-of-living-adjusted 1975 cap of $250,000 would have been $838,150. But, as I said, the cap had not been raised, and, in light of this, the cap had become so draconian that it had driven most personal-injury attorneys from the field, and the ones who remained, like Domecus, were forced to be very, very picky because they could not afford to lose. The margin for error had simply grown too thin for most of them to stay in that business.
It was possible that Ilene and I were not going to be able to find August any lawyer at all. And we were working against the clock: there was a seven-year statute of limitations. We had until 2006 to file a case. And we had just lost two years.
Throughout the 1980s and 1990s, states across the nation adopted laws similar to M.I.C.R.A., driven by the twin desires to protect doctors and hospitals from litigation and to please the general public, which wanted to see an end to “frivolous lawsuits.” Our national folklore about “frivolous lawsuits” was given great impetus when, in 1992, Stella Liebeck spilled scalding McDonald’s coffee in her lap and later sued the company, winning a big settlement and attracting a flood of negative attention. The press picked up on the multi-million dollar verdict but never reported that the judge in the case drastically scaled back the monetary award. This folklore helped shape the environment existing today in which it is virtually impossible for an injured patient (or his/her family) to sue for medical malpractice. In other words, the pendulum has swung far in the opposite direction from where it had been in the 1970s, 1980s, and early 1990s.
§
HERSH & HERSH, A SAN FRANCISCO LAW FIRM
After Lerch and Domecus, we found a third lawyer. This third one, like Goldilocks, we thought “just right.” By then we were in the middle of 2001.

Nancy Hersh, president of Hersh & Hersh
The brother of a former girlfriend, Wesley E. Overson, himself a successful San Francisco attorney, advised me that Nancy Hersh, president of Hersh & Hersh, was “very good.” So, I met with her in the late afternoon of Tuesday, July 3rd, 2001. She impressed me, and she agreed to accept our case. The firm took it on a contingency basis, contingency meaning that a fee would be payable only if there were a favorable result. She subsequently turned the case over to Charles Kelly, at the time a junior member of the firm. She assured me that she herself would oversee Charles’s work. Both she and Kelly had graduated from excellent law schools. They represented the best and the brightest.

Charles Kelly of the San Francisco law firm Hersh & Hersh
Kelly had to mount a case in spite of M.I.C.R.A. He was additionally tasked with successfully suing UCSF, a powerful institution, the largest employer in the city and county of San Francisco, and a commanding force in the region. It keeps a battery of lawyers full-time on its payroll to fend off suits like ours and has the deepest of deep pockets.
Kelly found an outside medical expert to review the birth records. Over the next year and a half, Kelly would inform us that UCSF was unable to produce the fetal heart monitor tracings (the birth’s paper trail), that this evidence had gone missing. He also told us that there was no mention in the birth records that the L & D nurse had alerted the resident to the baby’s low heartbeat at 2:55 a.m. Were we certain that this conversation had occurred? Evidently, Ilene and I were the only ones who claimed that it had. Pattye had been out of the delivery room at the moment it took place. There was even some lack of clarity about who the L & D nurse was, she being a per diem.
§
OUTSIDE MEDICAL EXPERT:
DR. JEFFREY GREENSPOON

Dr. Jeffrey Greenspoon, whom our attorney hired to serve as an outside medical expert to review August’s birth records. Greenspoon now works at CoxHealth in Springfield, MO.
Kelly would rely entirely on the finding of an outside medical expert he hired to review August’s birth records. This outside expert was Dr. Jeffrey Greenspoon, a physician at the time located in Los Angeles. Kelly must have taken for granted that someone living four hundred miles to the south would not know the defendant (Kilpatrick, et al.) and so could remain impartial as he reviewed the records.
During this period, Ilene and I were unfamiliar with Dr. Greenspoon’s background, and we didn’t question Kelly’s judgment. We believed that Kelly must know what he was doing. Moreover, we just assumed that, because he had a strong interest in winning the case, he would seek out the best possible medical expert.

The family, 2002
Greenspoon received the records of August’s birth in the middle of July, 2001. Our attorney did not hear anything definitive back from him until December of 2002, at which time Greenspoon reported that malpractice most definitely had occurred.
A trial date was set for November 8, 2004. Kelly flew to Jacksonville to prepare Ilene and me for legal depositions, which I believe took place in January of 2003. She and I were deposed separately in an office near the top of the Bank of America building in downtown Jacksonville. Each of us spoke at length about the low heart rate detected at 2:55 a.m.

August in 2003
But then, in the late spring of 2004, Greenspoon backtracked. He reported to Kelly that he had reviewed August’s birth records a second time and found a mistake. He’d initially thought the time of the birth to be 4:10 a.m. when in fact it had been 3:44 a.m. The time of 4:10 a.m. would have been outside the thirty-minute window opening at 3:33 a.m. However, because Dr. Kilpatrick had discovered bradycardia at 3:33 a.m. and delivered the baby by 3:44 a.m., he concluded that she had done nothing wrong and that UCSF was not at fault.
Kelly’s letter to us, dated June 28, 2004, informed us that Hersh & Hersh was no longer interested in litigating our case. Greenspoon had “re-reviewed the heart rate tracing [presumably for 2:55 a.m.] and believes that the heart rate seen on the heart monitor tracing is Ilene’s and not August’s.”

August in 2004
Kelly’s letter went on: Dr. Kilpatrick and Dr. Lipschitz discovered at 3:33 a.m. that August was in trouble, and they got him out by 3:44 a.m. They delivered him in eleven minutes, and that span of time was within the thirty-minute window, so the hospital was not at fault. The following sentence delivered the coup de grâce: “With all of the evidence establishing that August was delivered within 10 minutes [sic] of the bradycardia, we cannot establish that UCSF was negligent in its care and treatment of you and August.”
The last time we heard from Kelly was on August 24, 2004, when we received an unusually terse letter from him in response to our follow up questions. He obviously didn’t want to deal with us anymore.
Nancy Hersh and her protégée Charles Kelly represented our third and final attempt to seek redress and uncover information through the courts. The seven-year statute of limitations for birth-injury cases was beginning to run out, and because we were now living on the other side of the continent, we concluded that it would be very hard to locate a fourth attorney in San Francisco from such a distance. So, we gave up. After that, with regard to the legal realm, the rest was silence. Silence, that is, except for the holiday cards that arrived every winter for the next seven years from the law firm of Hersh & Hersh.
§
CONFLICT OF INTEREST
Dr. Greenspoon’s assessment didn’t seem right to Ilene and me, but then, who were we to question it? We weren’t doctors, we didn’t know, so we accepted the legitimacy of what the outside medical expert concluded. We were deeply disappointed by the news, but we just didn’t question it. Raising two small children, one of them medically high maintenance, did not give us time to think further about the matter.
After August died, I found that I had a little time on my hands, so I started poking around on the Internet in an effort to begin piecing together the narrative of his life. By this point in history, it had become remarkably easy to track down information. Additionally, I also now had access to my university’s databases, where ordinarily a lot of information would be hidden behind paywalls. I discovered that, like Dr. Kilpatrick, Greenspoon was a perinatologist. I also learned that, in the middle of 2001, when Kelly hired him, he was working at another medical school associated with UC: he was practicing medicine at the University of California, Los Angeles (UCLA).
The facts of his subspecialty and his affiliation with UC raised questions. UCLA wasn’t the only place Greenspoon practiced in the Los Angeles area, but it was one of them. First, would someone connected to UC be willing to find UC at fault? (Along with Kilpatrick, UC was one of the defendants named in our malpractice suit.)
And second, in the relatively small field of perinatology connected with medical schools, especially ones in the UC system, wouldn’t he have had to be aware of her? Wouldn’t he have crossed paths with her at academic conferences? And wouldn’t he have served as a peer reviewer on at least one of her many scholarly articles? Established and published, he himself was a figure of some significance in the field of perinatology. The articles for which he is listed as one of the authors came out beginning in 1985, and they continued to appear in the 1990s. Kilpatrick started publishing about a decade later than he did, and, in 2006, she joined the editorial board of the same journal that had published many of the articles to which Greenspoon’s name was affixed, the American Journal of Obstetrics and Gynecology. Greenspoon’s last article is dated 2001; she, on the other hand, remains prolific Her last came out in 2020. This doesn’t prove anything, of course, except that it’s a small world (after all). So, even if he didn’t know Kilpatrick first hand, he very likely had to have known of her. It would have been hard to miss her rising star.
The whole thing smacked of conflict of interest. I came to strongly suspect that Greenspoon in 2001 probably had known Kilpatrick personally and so should not have agreed to serve as an independent medical expert. But even if he’d never heard of Kilpatrick, he still should have disqualified himself based on his affiliation with the UC system.
Due to these findings, I began to question his and Dr. Kilpatrick’s accounts. Was it just a coincidence that his synchronized exactly with the one she had given in her legal deposition?
Dr. Kilpatrick had said in her deposition that she first became aware of a problem at 3:33 a.m. I am not charging that she lied under oath, but I am pointing out that this 3:33 time signature was not accurate. The most charitable thing one can say is that she misremembered the time. She had been informed at 3:03 a.m. about an irregularity with the baby’s heart rate. And I knew that she finally understood the severity of the problem at 3:42 a.m. How had I known? Because I was in the room where it happened, to alter a lyric from the musical Hamilton. As I said before, I saw the look on her face, the expression of extreme concern when she suddenly realized that the birth was going very badly.
Greenspoon’s and Kilpatrick’s accounts were in lockstep except on one key point: Kilpatrick had not mentioned in her legal deposition that Dr. Lipschitz informed her at 3:03 a.m. that there had been a problem with the fetal heart monitor at 2:55 a.m. In fact, no notes appeared in August’s extensive birth records touching on a conversation between Dr. Lipschitz and the L & D nurse at 2:55 a.m. about the EFM. Why, then, had Greenspoon gone out of his way to insist that the heart monitor at that moment was picking up the mother’s heart beat and not August’s? He introduced the subject apropos of nothing.
Crucially, Kelly had told us many months previously that the hospital had been unable to produce the fetal heart monitor tracings (the birth’s paper trail), that this evidence had gone missing. And yet, judging by the fact that Greenspoon had gratuitously interpreted it, he somehow must have come into possession of the tracings. How though could this have happened? I repeat: how could this have happened?
§
WHITE WALL OF SILENCE
Be that as it may, which, at this late point is all I’m left with, “Be that as it mays,” Greenspoon used the tracings to validate the opinion Kilpatrick stated at 3:33 a.m. regarding the heart monitor reading: “Yes, it must have been the mother’s.” And yet, with the benefit of twenty-twenty hindsight, Greenspoon should have been able to see that she had been wrong to corroborate the misreading that Lipschitz made at 2:55 a.m. when the latter claimed the heartbeat “must be mom’s.” Instead, he insisted that Kilpatrick’s confirmation of Lipschitz’s misreading was correct. Why do I say “misreading”? Because the catastrophic birth occurring forty-nine minutes later belied Lipschitz’s interpretation of the fetal-heart-monitor reading.
Looking back, it is difficult to understand why Kelly did not see that, in light of the terrible outcome, the indications were overwhelmingly on the side that the monitor had indeed been picking up the baby’s heartbeat. Why did he not see that Dr. Greenspoon’s assessment that the monitor was picking up the mother’s heartbeat was just a subjective opinion? Why did he not see that Greenspoon’s judgment was not rooted in empirical science? Why did he not see that Greenspoon’s reading of the data was, at best, how shall I say, “counter-intuitive”? To put all of this another way, why did Kelly not see that Lipschitz’s “must be mom’s” had swelled into a self-echoing, self-certifying chorus?
Not to put too fine a point on it, Dr. Greenspoon had covered up a colleague’s error, and Kelly didn’t catch it. I am not saying that Greenspoon deliberately lied, but I am speculating that he had an unconscious bias, preferring to believe the account of a well-respected physician over anything else.
Regardless of whether it was a deliberate lie or the product of unconscious bias, the outcome was the same. Before my son’s tragic encounter with the health care system, I had never heard the phrase “white wall of silence.” But I now believe that this must have been the wall August ran up against. August’s case had gone nowhere because of the white wall of silence, of physicians closing ranks to defend one of their own.
§
KILPATRICK WAS BULLETPROOF
Kelly neither suspected anything incongruous in Greenspoon’s finding nor broached seeking a second opinion–of locating another outside expert to review the records. Instead, he unceremoniously dumped us as clients.
In the final analysis, the fact that Kelly picked one UC employee to review the case of another UC employee, someone Greenspoon probably personally knew, indicates a profound level of incompetence. Having an expert who works for the same system (even remotely) review a case was patently ridiculous. It was ludicrous that any attorney would have thought that this was a reasonable way to pursue a case. Nancy Hersh had told me that she would oversee Kelly’s work, but, my guess is, she didn’t.
And yet, one factor remains that overrides Kelly’s incompetence. Dr. Kilpatrick, a nationally recognized expert in her field of perinatology, probably was bulletproof anyway when it came to lawsuits. It was going to be extremely difficult, nay, impossible, to find a medical expert willing to testify against her in court. Dr. Kilpatrick had a formidable reputation. Even so, Kelly should have found someone from outside the UC system, and probably from outside the state of California, to review the birth records. But, alas!
I gained a new understanding of what Dr. Kilpatrick had meant when she told Ilene at her six-week postpartum check that August’s terrible birth was “bad luck.” Yes, it WAS bad luck. It was bad luck for Ilene to have given birth under the supervision of a renowned perinatologist who was bulletproof.
The case continues to live on the internet. Go here: August David Chazan-Gabbard et. al vs. University of California Medical Center et. al
§
AFTERWORD (2012):
DR. GREENSPOON
After August died, I did some sleuthing with regard to Dr. Greenspoon and discovered that he came with a provocative back story. In 1995, he wrote a public letter to the pro-life Congressman Henry Hyde in which he passionately defended the controversial procedure known in medical circles as intact dilation and evacuation, or, what pro-life activists were calling partial-birth abortion. Greenspoon had stepped forward to defend a deceased colleague at Cedars Sinai Medical Center who had performed the procedure hundreds of times. In the mid 1990s, Greenspoon served as the director of a high-risk obstetric unit at Cedars Sinai in Los Angeles, the same medical center, coincidentally, where Dr. Kilpatrick is currently teaching and practicing.
Greenspoon wrote, “[a] pregnancy that is desired and planned is the foundation for the next generation of productive, healthy Americans . . . . The burden of raising one or two abnormal children is realistically unbearable.” His expertise on the subject of “abnormal” children, he indicated, came from serving as a speaker for a national Spina Bifida association.
In 2012 phone remarks made in an interview with Tucker Carlson (very far from my favorite commentator), Greenspoon stated that he approved of eliminating “babies who don’t have much of a viable life.” He went on to complain that it was unfortunate that the term eugenics had “somehow” taken on a pejorative meaning over time.
Here is a link to a Feb. 21, 2012, article in Slate titled “Eugenics, American Style” speaking about both Greenspoon’s public letter and Carlson’s interview; Greenspoon comes up at the tail end of the piece.
Go here: “Eugenics, American Style”
Greenspoon’s wording in his 1995 public letter and in his 2012 interview is infelicitous for several reasons, but I will focus on just one aspect. When it came to families he claimed he cared about, he certainly didn’t show any concern for ours. His reading of August’s birth records contributed mightily to increasing my family’s “burden of raising” a significantly impaired, or, in his phrasing, “abnormal” child. It made my and my wife’s task “realistically unbearable.” His reading of the birth records effectively thwarted the possibility winning a settlement, something our family desperately needed in order to care for our exorbitantly expensive child. We nearly went bankrupt as a result.
Greenspoon is currently practicing medicine at CoxHealth in Springfield, Missouri.
§
STORY MOVES TO JACKSONVILLE (2001)
August moved with his family to Jacksonville in 2001 so that I could take a tenure-line teaching position at the University of North Florida.
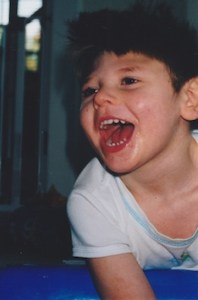
August on his wedge, 2004
Our daughter, Clio, was born in late 2001 at St. Luke’s Hospital, now called Ascension St. Vincent’s Southside Hospital. Unlike the first birth, this one went smoothly.

Ilene with August and Clio
Our son’s life was relatively peaceful in Jacksonville, where he attended the Mt. Herman Exceptional Student Center during the day. His health was extremely good between 2001 and 2010. Several years in a row he received a perfect attendance award. After school and during holiday breaks and the summer, he went to the DLC Nurse & Learn, where I now sit on the board of directors. (To see video and pictures of August, go here: A Boy Named August).

August with his sister Clio, born 2-1/2 years after his birth

Clio and August
§
SIGNIFICANT IMPAIRMENT
Back in 1999, when we were still living in San Francisco, one of August’s therapists–a friend–had written in a report that, on account of August’s brain injury, he had increased tone in all of his limbs, but decreased tone in his neck and trunk muscles. This combination brought about “severely limited active volitional movement.” Over the succeeding years, her assessment remained accurate. August couldn’t move his limbs, except for his legs, which he was able to kick, and his left arm, which he could flail. Moreover, he never improved intellectually. His developmental gap continued to widen. He was only going to make it to about a one-year-old level by the time he was an adult, if that. He was like a baby who kept growing bigger and bigger without any increase in skills and abilities.

August and Ilene, 2005

August rides a horse with Lisa Federico (hippotherapy)

August and Clio, 2010

August in his Africa shirt

August in his Muppet’s Animal shirt
MEDTRONIC BACLOFEN PUMP (2010)

Wolfson Children’s Hospital, Jacksonville FL.
On July 8th, 2010, a Medtronic Baclofen pump was implanted in August. The operation took place at Wolfson Children’s Hospital in Jacksonville, a teaching hospital associated with the University of Florida’s medical school.
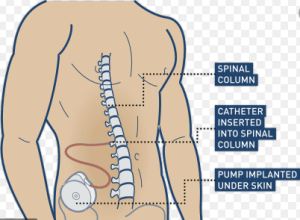
Medtronic Baclofen pump
The pump’s purpose was to decrease the spasticity associated with August’s cerebral palsy.

Dr. Hector James of Wolfson Hospital
Dr. Hector James implanted the pump. In 2003, he was recruited to run the first pediatric neurosurgery program in northeast Florida. A multimillion-dollar endowment made founding it possible. The internationally recognized Dr. James, originally from Argentina, had been practicing medicine for four decades, much of that time at a teaching hospital associated with the University of California, San Diego. Having recently retired, he had accepted an offer from the medical school at the University of Florida to come open a clinic at Wolfson Hospital.
He headed to northeast Florida to begin building a program, recruiting other pediatric neurosurgeons from around the nation. His name and reputation were the attraction. And this is how the area’s first Medtronic implantable infusion pump program came into existence.

Dr. Louise Spierre of Wolfson Hospital
Dr. Louise Spierre is one of the doctors Dr. James recruited to move to Jacksonville, and she was August’s physiatrist. From 2008 to 2010, the combination of oral Baclofen and Botox injections under her direction had been doing the job of controlling August’s spasticity quite nicely. But in late 2009 she changed her tune and started strongly advocating that we have a Medtronic Baclofen pump implanted. She told me that the pump was reasonably safe, almost as safe as riding in an airplane.
§
PERSUASIVE SALES PITCH
Over the course of several visits, Dr. Spierre and I talked about the Baclofen pump. At one in particular, a representative from Medtronic attended. Ilene was not present. She wasn’t able to come to most of these appointments. My employment at the university allowed me more flexibility than her job did. I could work late at night or early in the morning, whereas her patients had to see her during regular business hours. Working in a physical therapy practice she didn’t own meant that she was paid hourly. For each hour she took off from work, she had to cancel an appointment with a patient, and doing so meant not getting paid for that hour. Given our shaky finances due to the high cost of August’s care, canceling patients was not an option for us.
There was also the fact that in April of 2009 Ilene herniated a disc in her neck from lifting August. A surgeon implanted a titanium disc to replace the injured one, and afterward she was severely restricted in how much weight she could bear. As a result, she could no longer get August out of or into his wheelchair. Because I could easily pick him up, I had become the dominant parent when it came to appointments, pick-ups, drop offs, clothes changes, and so forth.
Dr. Spierre told me that afternoon that she had two effective methods in her tool kit for treating children with spasticity. They were the periodic off-label Botox injections with Baclofen daily by mouth, the regimen we were pursuing, and alternatively an implanted pump. The pump was an astonishingly high-tech innovation. The combination of Botox injections with oral Baclofen was the opposite: it was effective but low-tech. In the years since, I have come to appreciate that the term low-tech carries pejorative connotations.
During our conversation, and with the Medtronic company rep present, Dr. Spierre began nudging me to abandon the injections in favor of implanting a pump. Nothing in August’s medical profile had changed requiring the transition, but the ease of the pump was what she emphasized. I wouldn’t have to bring August into her clinic every three months for the next set of shots.
In her presentation she was upbeat, her voice inflected with optimism. The issue, she explained, was that when Baclofen is taken orally, most of the drug stays in the bloodstream. The targeted area for the drug was the cerebrospinal fluid (CSF) that bathes the spinal cord and the brain. When taken by mouth, only a small amount of it reaches the CSF, even at very high doses. Additionally, high doses of Baclofen are toxic to the body’s other organs, such as the kidneys and liver.
Speaking in a pleasant tone and projecting a ‘can do’ attitude, she said, “The pump bypasses these organs by injecting liquid Baclofen directly into the cerebrospinal fluid.” As she went on explaining the benefits of the device, I could tell that she really wanted Ilene and me to give up relying on Botox injections to manage August’s spasticity. She was pushing the pump.
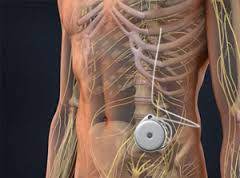
Dr. Spierre continued with what was turning into a sales pitch. She brought out a laminated card the size of a sheet of paper. Explaining the two diagrams on it, she walked me step by step through them. It was a color illustration of what the pump arrangement would look like anatomically, two angles of the same human subject, one facing forward, the other in profile. Visible in both the front and side views was a circular reservoir smaller than a hockey puck implanted under the skin of the two figures’ lower abdomen. A catheter then ran internally (within the body) from the reservoir in the front of the body around to the back, to the lumbar area (above the buttocks), entered the canal surrounding the spinal column and threaded within the canal up to about the midpoint of the thoracic spine (below the shoulders). There, within the spinal column canal, in an area called the intrathecal space, liquid Baclofen would emerge from the catheter tip in a slow drip and mix with the CSF surrounding the spinal cord. The CSF, with the drug Baclofen diffused into it, eventually would spread up into the CSF surrounding the brain, the target for the drug.
Laying the card aside, she said, “When Baclofen is supplied this way, the patient needs less of it, and this minimizes some of the drug’s negative side effects such as drowsiness, nausea, low blood pressure, and dizziness, not to leave out the drug’s toxic effect on the other organs.”
“There is also the matter of convenience. You will only have to come in once every six months. The Baclofen pump reservoir only needs to be replenished with liquid Baclofen roughly twice a year.”
She informed me that she or her physician assistant, Elsie Carrigan, would refill it subcutaneously. One or the other of them would insert a needle through the skin to the reservoir (located to the side of August’s lower abdomen) just below the skin’s surface and inject a fresh supply of Baclofen into it using a syringe. Setting the dosage of liquid Baclofen entering the patient’s spinal fluid would be regulated wirelessly via remote control. At this point, she showed me the remote control, and she let me hold it, but for no more than ten seconds, as though it were precious.
Dr. Spierre explained how the pump worked and described for me the long-term benefits, in essence what would be the payoff. “With reduced systemic spasticity,” she said, “August might be able to gain sufficient motor control to feed himself. With occupational therapy he may eventually be able to guide a spoon into a bowl and bring the food to his mouth. He won’t need to be hand-fed. Not at first, of course,” she cautioned, “but with occupational therapy. Immediately following the surgery, he would spend two weeks as an inpatient at the Brooks Rehabilitation Center here in Jacksonville.”
“With therapy,” she continued, “he should be able to walk more naturally in his gait trainer, as opposed to what he is doing now.” Currently he was thrusting himself forward with spasmodic, jerky motions, like a tin man needing oil.
“I don’t know,” I said. “The pump’s probably too expensive for us.”
“The Baclofen pump is not experimental. Your Blue Cross/Blue Shield insurance plan will approve the pump, its implantation, the two weeks of therapy at Brooks, and all of the follow-up. You have the PPO plan, right?”
I nodded, trying to take it all in.
“Good. It will cover 80 percent of these expenses, and Medicaid will pick up the remaining 20 percent.”
“Is the pump dangerous?” I said. “It seems terribly complicated.”
“These pumps represent a sophisticated approach to managing spasticity,” she told me. “They have been in common use for well over a decade. Dozens of children living in the local area now have them.” In essence, she was telling me that the pump was reasonably safe, almost as safe as riding in an airplane. Having a pump implanted in our son was just about worry free.
“But are they really safe?” I persisted.
At this point the Medtronic rep looked me straight in the eye and assured me that the pump was a safe product. If Ilene and I decided to go with it, he went on, he personally would accompany us “on each step of the journey.” Everything would go well—he would “make certain.” He would “see to it.”
When I spoke with Ilene that night about the pump, she was full of doubt. In fact, she flat out didn’t like the idea. She had been made cynical about medicine after having given birth to August in one of the world’s finest hospitals.
At the next appointment, when it was just Dr. Spierre, August, and I, the doctor didn’t want to dwell on the pump’s potential hazards. When I pressed her a little more, she conceded that there had been some problems when the pumps first came on the market over a decade earlier. But she reassured me, saying, “We’ve come a long way since then.” The only perils she would admit to were minimal and manageable, having mainly to do with the pump hardware having been known to malfunction or the catheter kinking. But about these problems she remained vague. How many pumps overall had the pediatric neurosurgery program implanted? She couldn’t produce a number. Could Ilene and I speak with other parents whose children had received the pump? No, we couldn’t: HIPAA (the Health Insurance and Portability and Accountability Act of 1996) prohibited giving out names, she said. How many pumps had the program been forced to remove, for whatever reason? She couldn’t say.
§
BRAVE NEW WORLD, À LA CARTE
Overall, what Dr. Spierre and Dr. James offered was terribly appealing. I trusted them because they were operating this university program through Wolfson Hospital—a children’s hospital and a beloved local institution. No one in the community doubted for a second that it was doing good and important work. To even suspect that the motives of its physicians or the institution itself might not be 100 percent honorable and altruistic would have been the equivalent of blasphemy.
I asked around about the pump. At Mt. Herman (August’s school) and the DLC Nurse & Learn, where he went after school, I mentioned it to one person after another, other parents and the teachers and staff. From them I detected muffled, generalized complaints. However, no specific game-changing horror story ever came to light. It was as if people didn’t like the pump, but they couldn’t say why. Nor could I find anything damning about the Baclofen pump on the Internet. I Googled repeatedly, using one set of search-term combinations after another, but nothing negative turned up. Had Jeanne Lenzer’s book The Danger Within Us: America’s Untested, Unregulated Medical Device Industry been published, or the Netflix documentary about medical devices The Bleeding Edge been released, I would not have allowed the pump to be implanted. But Lenzer’s book would not come out until 2017, and the documentary not until 2018–seven and eight years, respectively, in the future. Consequently, the premonitions of ill fortune were like household moths–it was hard to locate where they were breeding.
On the other side of the question were Dr. Spierre and the positive persuasion she brought to bear. She was a techno optimist, and her enthusiasm was infectious.
§
DR. STEPHEN LAZOFF

Dr. Stephen Lazoff not pictured, now retired
Dr. Stephen Lazoff, August’s pediatrician, advised us against implanting the pump. He has now retired to North Carolina, the place where Floridians go to retire, but when still working he belonged to a Baptist pediatric practice located just off San Jose Boulevard near Baymeadows in the Mandarin neighborhood. He was an older physician nearing retirement. I knew that he cared deeply about August. Back in 2001, when our family moved from San Francisco to Jacksonville, he had agreed to take August on as a patient in part because of our mutual Stanford connection. He had served his residency in the Stanford Medical Center, and I had earned my PhD in Stanford’s English department. But he also wanted August as his patient because he wished to accept the challenge that a boy like him would pose.
Ilene rearranged her busy patient schedule and managed to attend one of August’s doctor’s appointments. And so, late one sweltering afternoon in May of 2010, the four of us–Dr. Lazoff, August himself, and his parents–occupied one of the small examining rooms in the group practice. Ilene opened the appointment by explaining the reason why we had come. Dr. Lazoff then repeated her words slowly, was thoughtful for moment, then said, “Be very careful.”
Ilene and I stood there, waiting for more. Finally, Ilene said, “For me, as a physical therapist and a mom, the biggest selling point is that the spasticity is masking his function. And if he had the Baclofen pump and went to rehab at Brooks to maximize his function, he would have a chance to do more. We as his parents should let him have this chance to do all he can, to move and to communicate with us.”
Dr. Lazoff nodded as he listened to her.
“And the Baclofen pump,” she continued, “would help with all that pushing up into standing he does while in his wheelchair. He breaks straps and the foot pedals of his wheelchair doing this. He even once broke off his headrest. He would stay more comfortable in his wheelchair, when he is riding on the school bus and sitting at school and for feedings.”
Dr. Lazoff was taking all of this in.
“The Baclofen pump,” she went on, “would decrease the scissoring of his legs when we are doing diaper changes and when he is trying to walk in his Rifton trainer. It would save him from the ‘Charlie horse effect,’ which is just the spasticity tightening up his leg muscles.”
Dr. Lazoff asked, “Has the Charlie horse effect continued with the Botox injections?”
“Botox is managing it,” she said. “But Chris is August’s primary caregiver, and his having to go into Dr. Spierre’s office so often for the Botox injections inconveniences him. Because of the herniated disc in my neck, he has to do all of the therapy and doctors’ appointments. He goes almost every week to one appointment or another for August. And that’s on top of doing a lot of August’s morning and bedtime routine, his feeding, hygiene, dressing, and bathing. And that’s not to mention taking him to school every morning and picking him up almost every afternoon. That’s a lot of time out of his work week.”
What followed then was Dr. Lazoff’s sober appraisal. “Nothing is inherently wrong with the device itself, at least that I’m aware of at this time,” he said. “The problem is with the highly invasive procedure that implanting it requires.”
I broke in, “But if it can relieve his spasticity…” I thought Dr. Lazoff was being too cautious, too conservative. I added, “What could go wrong?”
“A lot can go wrong,” he said. He went on to say that patients of his who had entered the Wolfson pump program had experienced difficulties. “Major problems,” he said. “Whenever you go into the back like that, you run the risk of serious unintended consequences.”
“But they do work,” I insisted.
“The pump is an aggressive approach,” he said firmly. “It’s a highly invasive procedure. There’s a simpler one available that’s close to equally effective, and that’s the treatment Augie’s currently on—Botox. You do know, don’t you, that you can go on indefinitely using Botox and achieve the same therapeutic effect as the pump? There have been some adverse effects with Botox, but, if I had to choose between the pump and Botox, I’d choose Botox. The risk is negligible compared to the pump.”
“But the pump would be so much easier. I wouldn’t have to go into Dr. Spierre’s office every three months. I’d only have to go in every six months.”
“The pump is the impressive ‘go-big-or-go-home’ option,” he countered. “We don’t think well of ourselves if we don’t ‘go big or go home.’ We want the most aggressive solution there is. Anything less, we think, is half-hearted—we worry that we’re not doing all that we can. But in medicine, sometimes less is better.”
We all stood there silently for a moment, except of course for August. He was cooing as he sat strapped into his wheelchair and played with a toy secured with a bungee cord to the tray in front of him. Finally, Ilene said, “What are the things that can go wrong?”
“Infection is the main problem,” the doctor replied. “And problems with the back, the spinal column. A lot can go wrong when you go into the back. But any number of things. I wish I could tell you more. H.I.P.A.A. restrictions, you see, prohibit me from discussing specific cases with you. But, believe me, a lot can go wrong.”
I didn’t say anything, but I remember thinking, “If there’s an infection, they’ll treat it with antibiotics.” This thought would come to haunt me later when I would learn that infected pump hardware could not be easily cleansed with antibiotics.
§
A NON-VERBAL CHILD CAN’T TELL YOU WHERE IT HURTS
Dr. Lazoff then added that August was a particularly bad candidate for a pump. His non-verbal status, he believed, should disqualify him. Two days earlier, Dr. Spierre had addressed this very concern. She had underscored that August’s disabilities—his non-verbal status—should not keep him out of the pump program. She had said, “August has as much right to a pump as any typically developing child.”
But this day Dr. Lazoff pointed out that August, being non-verbal, wouldn’t be able to tell anyone how the pump was making him feel. And how and what he felt would be an important factor in helping Dr. Spierre find the right dosage of Baclofen. “The speed of the pump is how the dose is determined,” he informed us.
“Yes. It’s wireless,” I said. “They use a remote control. I know because she let me hold it.”
He disregarded this, then continued, “Without a verbal cue from the patient, how’s Dr. Spierre going to know at what speed to set it? Doing this right requires constantly adjusting the speed in light of the patient’s spoken response.”
“Clinical observation,” I said.
“But if Augie can’t tell her what or how he feels, I don’t see how she’s going to be able to do that.”
“Clinical observation,” I repeated.
“Will that be enough?”
“I’ve been told it will be.”
“But I don’t think it will. He’ll be a black box. By your own admission, Dr. Spierre is only going to see him once every six months. How can she possibly do any clinical observation if she hardly ever sees him? And you as the parents, how are you going to be able to judge? It will be up to you to perform the ‘clinical observation.’”
Ilene entered the conversation at this point, saying, “So you don’t think the pump is a good idea.” She was repeating Dr. Lazoff’s sentiment for the sake of clarity, to help herself absorb it.
Turning to her, he said, “I have seen so much go wrong.” I remember thinking, “If so much has gone wrong, why isn’t that information available on the internet?” I didn’t realize that, in three more years, stories of serious trouble would begin to appear there. In fact, starting in 2013 the pump would undergone several FDA class 1 recalls due to fatalities linked with it.
§
THE KILLING SEASON
After our visit with Dr. Lazoff, Ilene and I pondered the move deeply. Our son’s level of spasticity was great to the point that he was exceedingly physically impaired, and the Medtronic baclofen pump offered us an opportunity to lessen it. But it also presented the possibility of fucking up August’s body even more than it already was. And that was the dilemma we found ourselves facing. Because we wanted the best for our child, and because we did not want to leave any stone unturned, we finally agreed to follow Dr. Spierre’s recommendation, and so the pump was implanted. What drove my thinking in part was the belief that Dr. Lazoff was “old school” while Dr. James and Dr. Spierre were research scientists at medicine’s cutting edge. They represented the best and the brightest.
I wish I could appear before my younger self at that precise moment in time, slap him in the face, and tell him to take a different path. But that younger self is gone, and I will spend the rest of my days regretting the decision we made to implant the pump. We should have listened to Dr. Lazoff because the dangers he alerted us to–infection and problems with the back–did in fact came to pass. The Medtronic Baclofen pump turned out to be a disaster from the very start.
At 9 a.m. on July 8, 2010, Dr. James began the surgery that implanted the Baclofen pump to the side of August’s lower abdomen. On the day of the procedure, I did not speak with the Medtronic rep, but he was present in the operating room while the pump was being implanted, on hand to answer the surgeon’s questions and occasionally to tell him or her what to do. Company reps for Medtronic and other medical device makers, I was learning, frequently did this. People in this line of work, often without having much or any medical training, earn substantial six-figure salaries. The size of their salaries indicates how flush the medical device industry is.
After the surgery and the recovery room, August was wheeled in a hospital bed back into the room where I was waiting for him. We had been assigned to a room in Wolfson’s east wing on a floor known as Five East. He was still heavily sedated.
After several days of closely monitored convalescence at Wolfson, August was supposed to go, as a follow-up, for two weeks of intensive therapy as an inpatient at Brooks Rehab. Ilene and I had been led to believe that, during these two weeks, physical and occupational therapists would help August learn how to feed himself, as Dr. Spierre had suggested earlier, before the procedure. August, though, while still at the hospital, was experiencing so much pain that he could not undergo therapy. He cried and cried and cried. Because he was non-verbal, he could not tell us where the pain was or what was hurting him.
The decision was made (by whom exactly I don’t know) that he could not go to Brooks because his discomfort level was too great. So we took him home. When I wheeled him in during the first month of weekly post-op visits with Dr. Spierre, he often would be wailing at the top of his lungs. Struggling with the presence of a large foreign object in his body, he was crying in a way that I had not seen or heard since his first two and a half years of life. It pained me that he could not tell me what was wrong.
Ilene and I didn’t know that July is the cruelest month. The month can be considered cruel on account of the “July effect,” an increase in the risk of medical errors and surgical complications when medical school graduates begin their residencies. In the United Kingdom, a similar phenomenon is called “the killing season.” This is to say that early July is not the best time to have a major–or perhaps any–procedure performed in a teaching hospital. Dr. James himself had several decades of experience, but who knows with which intern-just-turned-resident he worked? Who knows who did what with August?
§
INFECTION & OOZING CSF
By late in the month of August, when our son was returning to the DLC and to Mt. Herman Exceptional Student Center for the Fall, CSF began oozing out of the incision site at the base of his back. When I saw it, I directly drove him back to the hospital. Dr. James informed me that the pump had become infected. Infection was a separate problem from the CSF dribbling out. So, really, there were two unrelated problems. In the following week, Dr. James performed a surgery with general anesthesia in an attempt to both disinfect the pump and stop the CSF leak. Because this effort was unsuccessful on both fronts, a third operation was undertaken. This one too didn’t work, so a fourth took place. And then a fifth.
In all, seven surgeries, each with general anesthesia, were carried out over a period of four months, starting on July 8th and ending in October of 2010. There were five hospitalizations, with the number of days of August as an inpatient totaling more than fifty. Most of the time August was assigned to a room on Five East.
I was learning on the fly just how frequently implanted hardware of one kind or another leads to infection. This would have been helpful to know before consenting to implantation of the pump. Dr. Lazoff had said something about infection, but I hadn’t grasped just how extensive, serious, and difficult to treat such problems were. Artificial knees, hips, shoulders, deep-brain stimulators, anything human-made that is put into the body is subject to infection. And once the artificial device turns septic, it is hard to disinfect because the synthetic material doesn’t respond to antibiotics in the same way that natural tissue does.
Slowly the realization dawned: I had done my research, but I hadn’t asked the right question. Months earlier I had gone online looking for information about Medtronic Baclofen pumps but hadn’t found anything negative. I thought that I was performing due diligence. But in addition to seeking information about pumps, I should also have been investigating the success rates of implanted hardware. Hardware infection in general was the issue, not the specific pump.
§
THE PICC LINE
“This next surgery will resolve the problem.” A faint Argentine accent whispered around the edges of Dr. James’s words. He said this several times, right before August was heading into yet another major operation. Each one to clean the pump was supposed to be the last. August would go in for a cleansing surgery, remain in the hospital as an inpatient during a recovery period, and then return home. Ilene and I would hope that the infection would abate. When it didn’t, we would head back to the hospital for another operation. Dr. James kept insisting that he could fix things, and, on his recommendation, I kept signing consent forms for further procedures. Ilene and I didn’t see any way out of this predicament. I know: it seems crazy. It is easy to look back now and question what the hell we were thinking, but we went along because we were in the fog of war. The doctor was telling us that our son needed these surgeries. To say “no” would have been like getting out of the endodontist’s chair in the middle of a root canal procedure. In contemplating the past, I don’t think it is an exaggeration to say that Dr. James became monomaniacal in his effort to cleanse the pump.
Most importantly, we trusted Dr. James and Dr. Spierre. I can’t stress that enough. Just as we’d trusted Kilpatrick, Lipschitz, Kelly, Hersh, and UCSF, we trusted these two doctors and Wolfson Hospital. And therein lay the rub.
So frequently was August a hospital resident that he had to have a peripherally inserted central catheter (or PICC line) put in. This was a long-term semipermanent central IV line entering his body on the right side of his neck. Having it there eliminated the need to stick IV lines into his arms or hands, where they would become detached with maddening frequency. It sometimes would take a nurse up to fifteen minutes to get a new “stick.”
Between surgeries, when he was at home with the PICC line, our house became a mini hospital, with the appropriate syringes, gauzes, and sterilization equipment laid out on a special tray. Four times a day, six hours apart, we had to inject antibiotic into his PICC line. This procedure had to be undertaken with extreme care. Not only did all the items have to be immaculately clean, but with each injection we had to avoid letting an air bubble creep into the fluid. A bubble could go directly to his heart and kill him. At least this was the extreme danger impressed upon us. Administering the 2 a.m. antibiotic was a nerve-racking experience. Knowing that a mistake could kill our child demanded focus. Going back to sleep afterward proved difficult.
§
“MOVE PUMPS”
Dr. James had a national reputation. Whenever I spoke with him, my voice became adenoidal, a little catch suddenly showing up in my throat. There was something paralyzing about being in the presence of this grandee of the house of medicine. Even so, moments occurred when the thought struck me that he was too old to be doing what he was doing. This thought slipped away when I saw the respect he garnered. One time, while waiting with August for our appointment to begin, an enthusiastic young male resident physician spoke with me. He was one of the residents among whom Joyce held court during rounds. The fellow now went on and on concerning Dr. James’s eminence. “It’s such a privilege to work with him!” he gushed.
However, other doctors at Wolfson were not so awestruck. During the times when August was an inpatient in the late summer and early fall of 2010, several of them approached me privately. Each one would preface his remarks (always a he) with something along the lines of, “You didn’t hear this from me ….” Each would took me aside and reveal sotto voce that implanting Medtronic Baclofen pumps often didn’t turn out well for patients. They also would inform me that trying to save hardware compromised by infection was futile. “It rarely works,” said one, and he went on to advise me to give up on saving the pump. One of them whom I will call Dr. Walker was colorfully emphatic: “That monstrosity of grandiosity needs to come out now.” These physicians intimated that a spirited debate was taking place behind the scenes. Dr. James’s manner of treating our son was being “hotly debated” within the hospital’s medical community.
The eighteenth-century British poet Alexander Pope wrote, “Who shall decide when doctors disagree?”
August’s body had become the site of a proxy battle. In other words, I inferred that bigger issues were at stake. Regarding what they were, I can only speculate.
This sort of sub rosa dissent kept surfacing. One of the main dissenters was a fellow I will call Dr. Munodi. One day, with the door of August’s hospital room closed–it was just the three of us present–he informed me that it was his opinion that Dr. James wasn’t properly weighing benefit versus harm. There could be secondary effects, he warned: a number of major surgeries conducted in quick succession like August was undergoing could initiate an unintended consequence down the line. On another occasion, Munodi speculated that Dr. James was trying to save August’s pump because he needed to prove something to his younger colleagues, who generally didn’t like him. It was obvious to me from Munodi’s tone that he himself didn’t. Keeping the pump in, Munodi asserted, was a matter of James’s pride mixed with generalized hubris.
During one of his short visits, Dr. Munodi asked me, “Did you come under any pressure to choose the pump over other options?”
“I don’t know,” I said. I stood there before him in August’s room, pondering, and then I suddenly felt dismayed. “I suppose,” I hesitantly answered. I’d never thought in such stark terms about that period when Dr. Spierre was advising me to switch from Botox injections to the pump.
“There has been some urgency to move pumps,” he muttered disapprovingly. “The hospital’s mark-up is considerable. The pumps are a profit center. The place is becoming a mill.” What he said reminded me of several lines from the Dire Straits song “Money for Nothing” about “moving” consumer products:
“We gotta move these refrigerators
We gotta move these colour TV’s”
Needless to say, Dr. Munodi’s words came as an unwelcome data point.
Years later in February 2013, Time magazine published Steven Brill’s 24,000-word article “Bitter Pill: Why Medical Bills Are Killing Us.” Reading it reminded me of what Dr. Munodi had said. Brill investigated hospital billing practices and revealed that hospital executives were gaming the system to maximize revenue. Reading that piece, I wondered if the pump had been prescribed for ulterior motives. It may have been the right mode of treatment, but, then again, maybe it wasn’t. Did the hospital and the university promote it out of self-interest? Brill reported that hospitals’ mark-ups for digital implanted devices (mechanisms such as Medtronic Baclofen pumps) were astronomical, serving as major sources of profit. Had Dr. Spierre, a university employee, been urged to prescribe more of them than she otherwise would have?
At the time I didn’t know what to do with what Munodi was telling me. I wondered why he, Walker, and the other men were backstabbing this great man. And I didn’t see the relevance to August’s care. Was I supposed to pick my boy up from his hospital bed and just walk out? Exhausted from the experience of staying long hours at his bedside, I simply didn’t have the mental bandwidth to process Munodi’s message.
§
“A HOSPITAL-PARENT SPECTER”
Dr. Spierre had said that August and I would be coming into her clinic about once every six months, but now I was hunkered down in the hospital for long hours every day. The herniated disc Ilene incurred from lifting August kept her from being on hand more. So, I became what Vicki Forman in her memoir This Lovely Life calls “a hospital-parent specter.”
I quickly discovered that I could not sleep for more than forty-five minutes at a stretch anyway, so I started driving home every night and returning to the hospital around 6:15 a.m. the next morning. Ilene would spell me for a few hours whenever she could, but her fixed work schedule made her unavailable during weekdays. She also had our young daughter Clio to look after. So, I lived for the most part at the hospital, preparing classes and grading papers by August’s bedside and only leaving to drive to campus to teach or home to sleep.
The operations were brutal for August and hard on Ilene and me. Because the University of North Florida (UNF), where I teach, at the time offered no paid family leave, and because Ilene and I were not able to take time off from work, we couldn’t be on hand during some of the surgeries. So we had come to rely on Katrina Johnson, who stayed with him during the day to keep him company while I was teaching. Often the procedures took place when I had to be in the classroom, so Katrina would be on hand to take care of him when he came out of an operation. When we first hired her, she was a UNF student, and for about six years she worked as August’s principal caregiver. She grew to love him like a brother, and August in return loved her. We considered her family, and so having her at the hospital was like one of us stay with him. Often she was the one present when he awoke from the anesthesia. In the post-surgery phases, she’d had to hold his head up as he vomited into a towel.
When the infection persisted after the fifth surgery, a sixth one was performed to remove the pump. And then, because CSF would not stop seeping out of the incision site, a seventh one was undertaken to address that problem. When the seven surgeries were over, August’s lower back was a crisscross of permanent, three-dimensional scars.
Right after the seventh surgery, Dr. James told me that he had done “something special” to bind up August’s back internally so that the oozing would stop, but he didn’t elaborate much concerning what this had entailed.
§
“A RIDDLE WRAPPED IN A MYSTERY INSIDE AN ENIGMA”
Something exponentially more serious than any problem we had ever witnessed before–something grotesque–started occurring in November of 2010, less than thirty days following the last of Dr. James’s seven surgeries.
August began arching. Arching, also known as extension, meant that, for periods lasting from up to ten days, August would involuntarily bend backward and to the side in a twisted position and remain in it. His limbs would be distorted, his back bent, as if perpetually trying to glance over his shoulder at his heels, causing him to resemble a human pretzel. For days on end he would be stuck in this contortion. In ballet, there is a pose called attitude derrière, and August sort of looked like that except that his leg wouldn’t be up in midair, his head would be permanently cocked to the side, and he couldn’t get out of it. “Fixity of posture and muscular rigidity” was how this condition was clinically described. External stimuli didn’t seem to bring on an episode, so we had no idea what event, if any, would trigger one. For the next three years, arching became, like Russia for Winston Churchill, a “riddle wrapped in a mystery inside an enigma.”
Because August was non-verbal, he could not tell us where the pain was or what he was feeling.
Did the arching result from the succession of seven operations August had undergone over four months? Did it come from something undertaken in the last of them? The sixth surgery had removed the pump, but CSF had continued oozing from the incision site at the base of the spine. So, Dr. James had performed the seventh and last to stop the leak. Afterward, he had told me that he’d done something special to get the job done. There was a seal, a patch of some kind.
During this period, neither Ilene nor I had the slightest idea what was causing August to arch. After his death, which stemmed from the arching, we developed more focused questions. Did the seventh surgery inadvertently inflict neurological damage? What was the “something special” Dr. James spoke of? There was a seal, a patch of some kind. Could he have patched the site of the leak too tightly? Was any part of a bone in the spinal column removed, leaving a sharp edge? Or did the surgery cause scar tissue to form in or around the spinal cord? Or, in tightening the dura, did Dr. James overdo it, inadvertently creating a tethered cord?
The arching was serious and intensifying. Frantic, Ilene and I decided to have a second Medtronic Baclofen pump implanted, hoping that it would alleviate the arching. Dr. Spierre told us that it might do just that. Actually, a lot more reasoning went into this decision than I am describing. The first pump, after all, did do what it was supposed to do–relieve spasticity. The pump itself was not the problem; the issue had been infection and the multiple surgical attempts to disinfect it. I know: today, looking back, putting in a second one seems crazy. We opted for it because the doctors weren’t suggesting any alternatives, and we were desperate. We didn’t know what else to do. Should we have had a second one lodged in his body? Ultimately, with regard to the outcome, it made no difference one way or the other.
Dr. Philipp Aldana of the pediatric neurosurgery program, a much younger man than Dr. James, implanted the new pump in the summer of 2011. This operation went without incident. No infection or other complication ensued.
The second Medtronic Baclofen pump gave everyone an opportunity to see what it could do to enhance August’s abilities. When first pitching the pump, Dr. Spierre had suggested not only that August would walk more gracefully in his gait trainer, but also that he might be able to feed himself. But, with the second pump, attempts to help him do either of these activities made no progress at all. After a number of months of working with him, the occupational therapists at Mt. Herman told me that the pump had done absolutely nothing to improve his prospects. If anything, the pump had made things worse. No possibility in the foreseeable future existed that he would be able to feed himself. The same was true for walking. Before the first pump was implanted, August used to gleefully tool up and down our long driveway in his gait trainer. Which is to say, he covered a lot of ground. But after the first pump was put in, he stopped walking, only occasionally taking a step or two. After the second pump, he never took so much as a single step. Like a statue, he would just stand motionless for long periods, a happy figure cooing in the breeze. And so, not surprisingly, the golden visions Dr. Spierre had conjured up about what the pump would do vanished into thin air.
As before, the Baclofen pump relieved August’s spasticity, but it did nothing to stop the arching.
§
“DOING HARD TIME IN THE BOWELS OF AMERICAN MEDICINE”
In the middle of 2012, Dr. Spierre began to suspect that perhaps the pump catheter was leaking or damaged or kinking and that maybe one of these had something to do with the arching. So, yet another major surgery was scheduled, a procedure known as a catheter revision. It would replace not the pump itself but only the catheter that snaked up his spine. This was the line that went from the pump on the side of August’s lower belly around his body to the base of spinal column and then upward to a point about midway up his back. So, on the morning of August 1, 2012–Ilene’s and my twentieth wedding anniversary–the neurosurgeon Dr. Aldana undertook the procedure.
During this surgery a change was made without our permission. Before the catheter-revision surgery, the tip of the catheter in August had stopped midway up the thoracic spine. After the surgery, it terminated in a new location, one much higher. Dr. Spierre had instructed Dr. Aldana to raise the tip to the second cervical vertebrae, C2, right below the skull. This was supposed to allow the benefits of Baclofen to be distributed throughout the greatest extent of August’s body.
Dr. Spierre hadn’t asked for our consent for this change. She didn’t inform me until the day after the surgery, so I hadn’t known about it during Ilene’s and my very short anniversary celebration. When Spierre told me, I didn’t think much about it. But when I mentioned it during one of my frequent cell phone updates to Ilene, she became livid. She didn’t like not having been consulted, she would never have approved, and she feared that it would lead to a terrible consequence.
And this is indeed what happened. A few days later I brought August home from the hospital, and, as Ilene had predicted, the unthinkable occurred–what had been a very bad situation became even worse. August’s arching suddenly, dramatically, astronomically increased to a new level of wretchedness. What had been mere arching became arching in extremis. Overnight it became orders of magnitude greater, going from grotesque nightmare all the way to the macabre. Like some figure out of Ovid, our son had metamorphosed into a twisted tree trunk of a boy, wrapping around himself, all kinks and swirls. August’s neck had become so bent that he couldn’t take anything by mouth. I had no way of getting food or drink into him. Whatever he did swallow he instantaneously projectile-vomited, something he’d never done before. In the state he was in, he was going to starve to death. And, on top of everything, he was crying, crying, crying. At my wits’ end and terrified, I decided to take him to the ER. His torso was so deformed, though, that I could barely strap him into his wheelchair. Once I finally managed to do that, I drove him to Wolfson Hospital.
August spent sixty-four straight days in Wolfson, twisted up into an Ovidian myth. In the Fall of 2012, he and I were living once again on Five East. It felt as though the Fall of 2010 had never ceased. We were back in the implacable routine of hospitals. Everything from two years earlier flooded back: the rhythms of hospital life; the bells, beeps, and intercom pages; the sound of wheels and knocks at the door; the odors of physicality. All of these quickly became mind-numbingly familiar. Interruptions to my grading of student papers were as common as cannabis dispensaries in Oregon. The main difference I saw between 2010 and 2012 was that the nurses had gone digital. Before, most everything had been done on paper. Now, the nurses did their charting on laptops placed atop carts they rolled from room to room. Seeing that August and I had returned, one of them joked, “You better not try and escape.”
August endured his days in bed and was turned periodically to prevent bedsores. Beneath him a thin but active electric air mattress hummed. The railings on each side always remained raised to prevent him from tumbling out. Small electronic monitors perched gargoyle-like above him, and they displayed colorful, squiggly, moving lines. These announced his rates of heartbeat and oxygenation, the metrics of his helpless little being. At least once every hour or two the electrodes attached to his body or the pulse oximeter gripping his finger would loosen. A noisy beeping would ensue and not be silenced until a nurse came, and sometimes that would take as long as fifteen minutes. Occasionally the monitors would go off for no apparent reason, to the same effect—a long wait for a nurse to quell the beeping.
Every day was a roller coaster of emotions, highs and lows, creating chronic nervous stress that no doubt was putting my own health at risk. During this period August and I communicated with each other in our own special language, and we listened to each other’s silences. But as the weeks dragged on, the wordless speech ran dry. Of the two of us, at least he remained cheerful.
We couldn’t find our way to the exit. Being caught in the health-care system is like being trapped in the legal system, especially if a child is involved. Once the bureaucracy ensnares you, you can’t simply walk away. You must play by its rules. So August and I were, as Doron Weber says of himself and his son Damon in his 2012 book Immortal Bird, “doing hard time in the bowels of American medicine.”
§
THE KANGAROO PUMP AND THE FEEDING TUBE
Because of the arching, it had become almost impossible for August to take food and water by mouth. The hospital’s main pediatric surgeon, Dr. Nicholas Poulos, surgically implanted a G-J (gastrostomy-jejunostomy) tube so that his amount of nutrition could be increased. Dr. Poulus trusted me with his personal cell number and took my calls when I needed to speak with him. His own child had spent months in this same hospital, and the way he acted toward Ilene and me indicated that he understood what we were going through. He represented Wolfson Hospital at its finest.
August thus became wedded to a machine: he required continuous enteral feeding. An artificial opening had been created at his abdomen. This opening had two ports, the G-port (for medications going to his stomach) and the J-port (for nutrition—PediaSure—going to his jejunum, the middle part of the small intestine). We had to stay focused: medication went into the G-tube, liquid nutrition into the J-tube. Mixing this up would bring serious consequences.
Most of the day and into the night, August had to be fed this way. Every few seconds, a pump would inject a spurt of PediaSure through a transparent plastic tube to the J-port and then into the jejunum. This was called J-tube feeding. A small blue-and-white pump called a Kangaroo was the injecting mechanism. Slightly smaller than a brick, it attached midway up on an IV pole. With this nearly around-the-clock feeding, the sound of the little blue pump turning on and off every few seconds, with a several-second delay between each burst, was like white noise broken up by a predictable ripple. Hummmmmmm-click-grrrr! Hummmmmmm-click-grrrr! Hummmmmmm-click-grrrrr! This sequence of sounds provided a constant and hypnotizing rhythm to our lives.
§
THE TOWER OF BABEL
More than two dozen physicians trooped through his hospital room to have a look. Inquisitive faces would approach the subject in his bed and peer down. Not one knew what to say. Not one suggested a name for the condition. Not one said he or she had seen it before. Not one had the slightest idea what the problem was. Not one seemed to have the slightest idea what to do.
Memories of two doctors in particular stay with me. One was a young, bantering male clinician, who said with witty aplomb, “Wow! That can’t be comfortable.” He delivered this wisecrack while viewing my boy all twisted up into a pretzel. The other was a raven-haired young female physician who chided, “What is wrong with you!? You are a parent in denial!” Wagging her finger furiously, she sharply informed me that I was a parent unable to come to terms with the fact that my child was “suffering from cerebral palsy.”
I believe I overheard about this time that the cost of our son’s care was running north of a quarter of a million dollars. If this was true, I’m surprised the figure was so low.
Every doctor who weighed in on the matter did so from the perspective of his or her specialty. The gastroenterologist thought the arching might be the result of “GERD” (gastroesophageal reflux disease). The orthopedist suggested the extreme solution of “rodding”–inserting titanium rods into August’s crooked back to keep it straight (although, to be fair, he himself didn’t like the idea). Each clinician who August and I dealt with was functioning on his or her own—cowboy style—consulting with other physicians only on an ad hoc basis. It was wormhole thinking. Each approached August’s case through the eyes of his or her specialty; each was in a silo, separate from the others, and each had the one-tool approach that comes with specialties, so that, overall, August’s care was fragmented. It was as if they had all had collectively decided to turn the field of medicine into a massive medieval passion play re-creating the Tower of Babel.
§
“PALLIATIVE CARE”
I had always looked favorably on palliative care doctors. Only a truly sensitive and caring person, I assumed, would take up such a specialty. And I still believe this. I would wager as an uneducated guess that over 95 percent of them are genuinely good, caring, sensitive people because it takes a special type of person to do that kind of work. But, as it happened, we ran into one of the few bad apples. Dr. Kelly Komatz seemed to have an agenda all her own. The first time she entered August’s hospital room, her mind was already made up. Even before reading his chart, she knew what to do. Within minutes she began lecturing me as though from a script.
“Have you begun to think about the next phase of his life?” Standing in her white lab coat, she intimated that I should start picking out a coffin. This question’s practiced quality indicated that she asked it a lot. A clinician with magical powers, she then got out her pad and started scribbling prescriptions. This physician was promiscuous with the prescription pad. These were pharmacy orders for dark potions and soporific elixirs. The Komatz cocktail consisted of morphine, Hycet (hydrocodone-acetaminophen), Neurontin (gabapentin), Valium, and clonidine, all to be started at once and together. Eventually, without subtracting any of these, and without explaining why, she added methadone.
The massive drugging did nothing to alleviate the arching, which was the problem that needed solving. Her potions didn’t do anything except keep August snowed. It couldn’t have been pleasant. And sometimes there were paradoxical responses in which, instead of being sleepy, he became agitated. But most importantly, the more the doctor drugged him, the more a chain reaction set in. One by one the physicians at Wolfson stepped back and checked out. If Dr. Komatz had been called in and was giving August a maximum of drugs, he must be dying.
§
THE DNR
Like the other physicians, Dr. Cliff David, who lived in our San Marco neighborhood, wasn’t able to solve the arching riddle. (Dr. David has since left Wolfson to move to North Carolina, where is now battling cancer.) August was noisily playing with a toy when Dr. David came into his room. Speaking slowly, David said that Ilene and I should figure out what our end-of-life wishes would be for August. What would we want the hospital to do if a life-threatening situation arose and one of us was not present?
“Life and death,” I said.
He looked at me sympathetically but did not speak.
“What life, what death?” I said.
“It would be good for us to know what the wishes of the parents are.”
Our wishes? Wasn’t this topic premature? How could death be the topic when the patient was busy thrashing his toy, the Activity Atom? I couldn’t wrap my mind around the two ideas at once: August playing, August dying. The two ideas were as incongruous. Once the subject had been broached, however, Ilene and I had to follow through. We wanted to be responsible parents. What would we want the hospital to do? Very late that night, we discussed the matter. Given our schedules, even this conversation had to be rushed, and we held it while brushing our teeth.
Central to our decision, when we reached one, was the wish that August not suffer. A feeding tube was one thing, acceptable in the big scheme of things, but a ventilator was quite another. We did not want him to be put on one, not if there would be little chance of him ever coming off it. We didn’t want him to endure pain by being kept alive if the only reason for sustaining his life was that we couldn’t let go of him.
The following day, before he went off shift, Dr. David helped us put our names to a “do not resuscitate” (DNR) order. (This directive has since been renamed an AND—“allow natural death.”) Ilene and I met with him in the late afternoon. We hovered and agonized over the document.
“I want to make certain,” Ilene said, holding the pen, “that August will continue to receive the same level of care he is receiving now.”
“He will,” said Dr. David.
“If signing this form means there’s going to be a change in his status or a drop off in his care in any way, I don’t want to sign,” she said. “Will he be treated the same?”
“Yes,” Dr. David assured her. “His status will remain the same. He won’t be treated any differently just because you have signed a DNR.”
Ilene hesitated for a long time, mulling it over. Finally she said, “Okay then. If nothing is going to change. We’re only signing this document in the event of the worst of a worst-case scenario. I don’t want the doctors or the nurses or the staff or anyone to lessen their care because we’ve signed this form. We believe that he will recover if he is given proper care.”
“Nothing will change,” said Dr. David reassuringly.
So she signed it. And I did too. And we had copies made to take home with us. This DNR order became like the handle on an airliner’s emergency exit door. We didn’t expect to ever have to use it.
Dr. David meant well, but August’s de facto status did change. It was a subtle difference. It was as if his hospital room had sprung a slow leak of oxygen. In the same way that everyone interpreted Dr. Komatz’ intervention to mean that August’s end was nigh, so it was with the DNR. This was especially true of the nurses. The DNR apparently depressed them—they seemed more somber knowing that it was in his chart. The nurses emotionally stepped back, preparing themselves for the worst. And I don’t blame them—the deaths of children are hard on them. No one wants to see a child die.
§
BLACK MIRROR
Eventually, August was released from the hospital in very late October, 2012, arching as ever. The doctors had been unable to do anything to improve the situation.
For us, the Medtronic Baclofen pump had been a horror story, an episode worthy of Black Mirror, the British television series using individual episodes to explore near-future dystopias utilizing science fiction technology. The difference was that, for us living the narrative, there was no fast-forward button to push past the awful parts. We had to live through every dreadful second of it. Ever since the implantation of the first pump in 2010, August’s bedroom had become the scene of crisis after crisis. Excitement, panic, and adrenaline rush had occurred at the worst part of each turn of the cycle. And the wheel just wouldn’t stop turning. Our world would become anxiety-laden and frantic as we struggled to deactivate the bomb that had been planted inside of our son.
Ilene and I were alone. And we acutely felt the accuracy of item fifteen on Roy Ellis’s 30 Signs You May Have a Disabled Child: “It dawns on you one day you know more than your doctor.”
This video shows what the condition looked like. Warning: it is difficult to watch.
/ Alternative link /
§
DYSTONIA
August was back in the hospital in the Fall of 2013 for the same reason. But this time the arching was making it difficult for him to breathe. On this occasion he was not assigned to Five East but to the sixth floor of another part of the hospital.
It was October 14th, 2013, a Monday. Disenchanted, I now wanted the second pump out. I became a man with a mission, convinced that it was going to kill August. That morning I spoke to the floor’s attending physician and anyone else who would listen. I asked, requested, commanded, ordered, implored, entreated, beseeched, and then begged that it be removed. I was a man running around with his hair on fire. I’m surprised now that no one called security. The attending physician tried to settle me down. He cautioned me that, given his state at the time, August couldn’t be operated on anyway.
Years later, in a 2014 TED Talk, “What Your Doctor Won’t Disclose,” Dr. Leana Wen stated that, for medicine to work, patients have to be able to trust their doctors. When the trust is gone, all that’s left is fear. All I felt now was fear.
In the middle of that afternoon, Dr. Spierre came from her clinic, blowing through the door like a bitter wind, eager to reconvert an apostate.
Samuel Johnson wrote, “There are a thousand familiar disputes, which reason can never decide.”
Ever since November 2010, Dr. Spierre had dismissed the arching as a problem that she didn’t cause, so it wasn’t hers to solve. Now, she and I found ourselves facing one another, she and I on opposite sides of August’s bed.
“He’s going to take this pump with him to the grave,” I predicted.
“Pardon me?” she said, eyebrows raised and staring at me.
“The pump has to come out.”
“Removing the pump will do nothing to resolve the arching,” she said calmly.
“No, I want it to come out. He’s going to take this pump with him to the grave!” I repeated.
She looked at me hard, baffled that I was being uncooperative. For about twenty seconds we remained silent. “Removing the pump won’t change anything,” she finally said.
“He’s going to take this pump with him to the grave,” I said a third time.
“Why do you keep saying that? Removing the pump out won’t solve the problem.”
“Because,” and then she leaned over the bed railing and waved her hand over August’s distorted form, announcing, “this is dystonia.”
I will never know why she waited until that moment to drop this bomb. Dystonia itself meant nothing to me; the issue was that—at this critical juncture—she suddenly and opportunistically had an answer to what August’s problem was. Whatever her reason for saying this word now, I was confounded, and the sensation came back of feeling a first shudder of the San Andreas. Dystonia was a new word. Dystonia. It sounded like dystopia. The two could form a rhyme in a poem.
Why had dystonia—whatever it was—never been mentioned to me before? August had been arching off and on for nearly three years. In summer of 2012, he had spent sixty-four days in Wolfson, twisted up into a jumble. More than two dozen physicians had trooped through his hospital room and viewed his arching. Not one of them though had pronounced the word dystonia.
I used to speak meekly to the doctors and nurses while Ilene was in labor at UCSF and later to Dr. James and Dr. Spierre because I revered members of the medical profession. But that reverence and meekness were now gone.
“What is happening?” I said.
She looked at me blankly. “What?”
“Why did you wait until now to tell me this?”
“What do you mean?”
“Dystonia,” I said. “You waited.”
“Waited?”
“How long have you known? You waited until I wanted the pump to be removed to tell me that his condition was dystonia.”
“No.”
“Hell, yes. I see it now. If I hadn’t forced your hand, you would’ve never said anything.”
“I don’t know what you mean.”
“How long have you not said anything?”
“I don’t know what you’re talking about.”
“How long have you been hiding this ace up your sleeve?”
“What are you saying?”
“How long were you planning to keep this concealed?”
“We haven’t concealed anything.”
“How long have you known?”
“I don’t know what you are thinking, but you’re wrong.”
“I suppose it’s just serendipity,” I said. “For three years he’s arching himself into a knot, and you don’t know what the hell his problem is. You lead me to believe it’s not your problem to solve. You say, ‘Let the neurologist–Dr. Abrams–deal with it.’ But now Ilene and I want the pump removed, and all of a sudden you know what his problem is. It’s dystonia.”
“It took time to diagnose.”
“Three years? Give me a fucking break! You expect me to believe that?”
“This is dystonia,” she said, trying to maintain her composure. “It’s a movement disorder in the same family as Parkinson’s disease.”
“Yes, okay. What now?”
In a low voice she said, “There’s a dystonia clinic operating at the University of Florida medical school in Gainesville.” Gainesville was sixty miles away.
This information took a moment to register. And then I was thunderstruck.
“What? You’re fucking kidding me, right? There’s a clinic within driving distance? A clinic nearby? But no one thought to tell us about it? There was August, arching for all to see, off and on for almost three years, displaying this condition before an army of medical professionals, living a life in hell, and it didn’t occur to you or anyone else to inform us that his condition was dystonia and that there’s a clinic nearby?”
“No,” she said, “you have it all wrong.”
“No. I don’t have it all wrong. What is there here to be wrong about! You haven’t done the best you could do for August.”
“We’ve done the best we can do.”
“Like fuck you have! Do you not see what you’ve done? Can’t you see? You’ve destroyed him. You’ve destroyed my son!”
“Calm down! Get a grip on yourself. We’ve done—”
“You’re the one who talked me into this.”
“Wait! What? No! The pump was indicated based on the patient’s medical profile.”
“This pump was your idea!”
“I encouraged you to consider the pump because it was the better of two options.”
“The pump has been a fucking disaster! I wish we’d never met you or that scrofulous shitbag, Dr. James.”
“The pump has nothing to do with what is happening now.”
Dumbfounded, I stared at her in disbelief. Below and between us lay August’s perversely twisted form, a vision straight out of the book of Revelation. He looked wan and tired, too frail and exhausted by this point to want to play with his favorite toy, the Activity Atom, which sat inert beside him on the sheets.
“As I’ve told you many times,” she said, “there is no way that the pump can be implicated.”
“There is no way that the pump can be implicated,” I repeated in mockery. “And while I’m on it,” I said, slightly changing the subject, “the one lesson you should take away from this sorry episode is this: you should never again implant a Baclofen pump in a nonverbal child.”
I’d struck a nerve. Dr. Spierre stepped back, as if stung by the charge, and then said in an icily adversarial tone, “His being nonverbal has nothing to do with any of this.”
“He was a bad candidate from the start,” I said. “But you needed patients.” And that was pretty much the end of the conversation.
And so, just hours before he died, Dr. Spierre finally diagnosed his condition as dystonia.
§
OCTOBER 15th, 2013
August was scheduled for discharge the next morning, Tuesday, August 15th. That Monday evening, Katrina arrived at six to watch him in his hospital room. I went for a jog. Already that day he had shown considerable improvement, and I assumed that things were on the mend. Having a lot of grading to catch up with, I prepared to go home.
August was lying in the hospital bed wearing a Reese’s Pieces orange T-shirt and a diaper. Arching as ever, he was now batting away again at his noisy Activity Atom and giggling. And then I heard it, his laugh.
Katrina said, “What’s so funny, Augie?”
I felt relieved. It was a sign that he was feeling better.
At 7:45 p.m. I left him in Katrina’s care. I exited the building under moonlight: a waxing gibbous moon had passed the zenith. Before I departed, August’s night nurse assured me that she’d watch closely over him. When I was pulling out of the parking lot, I suddenly remembered that I’d forgotten to give August a kiss goodbye the way I usually did before leaving. I’ll give him an extra kiss tomorrow morning, I thought as I drove away. I planned to return a little after six the next morning, Tuesday, to get him ready to go home.
Katrina remained with August until after he’d fallen asleep. That was at 10 p.m.
At a little past midnight, Ilene and I had just fallen asleep when her cell phone rang. She answered, and someone on the other end told her that August was having trouble breathing. We decided that I should go back to the hospital and that she would remain behind with Clio, who was asleep and too young to be left alone in the house.
I took the elevator up to the sixth floor. A broad, well-lit corridor appeared when the elevator doors opened and, beyond it, a set of white double doors secured against intruders. Someone on the other side, at the nurses’ station, pressed a buzzer to allow me in. I rushed to his room, and there he was. I knew without delay that this was the beginning of the end. In the sight of him there was no bode of dawn.
I called Ilene. Our neighbor across the driveway, Suzanne Honeycutt, came over to stay with Clio, who remained asleep. Ilene soon arrived, and we assembled in the same room where hours earlier I had said to Dr. Spierre, “He’s going to take this pump with him to the grave.”
The little Kangaroo feeding pump had been turned off. August was unconscious. In his contorted posture, he hadn’t been able to clear his fluids. His breathing now was exceedingly labored. This was the death rattle I had heard when Dad lay dying nineteen years earlier.
Although we could have, Ilene and I didn’t request that August be placed on a ventilator. The attending physician, someone I will call Dr. Choudhury, a young woman from India, didn’t try to change our minds. She asked if we wanted him to be given morphine. We did. Morphine impedes respiration. August’s breath came slower and slower.
“I switched to pediatrics,” Dr. Choudhury said, tears welling in her eyes, “to avoid scenes like this.”
It was strange to be with our son and not hear the Kangaroo, so accustomed to its sound had we become. We couldn’t tell how much consciousness remained, so Ilene and I took turns whispering in his ear.
In his ending was his beginning. At nearly the same hour of the early morning that he had been born fourteen years earlier, he died in our arms. We laid him on the bed, and Dr. Choudhury lifted his left arm from the linen and held it at the wrist. A large-faced analog clock was mounted on the wall behind her. She glanced over her shoulder to note the official time, announcing in a neutral tone, “2:20 a.m.”
§
THE YEARS FOLLOWING

Clio dispersing August’s ashes at Tennessee Valley Beach, Marin County, CA, July 12, 2014
The morning August died, Ilene and I broke the news to Clio. It was still the early morning. She was eleven, two weeks short of turning twelve. She was in her bed, and when she understood what we’d said, she bolted up and ran wailing through the house to his bedroom. There she threw herself down on his empty bed and howled. And there she remained a long time.
Ilene’s sense of loss was and is well beyond my poor powers to describe.
§
THE RIDDLE SOLVED
In 2015, Ilene came home from her physical therapy practice, the one she had come to own, Ergo Body in San Marco, and told me that she had had an interesting conversation with one of her patients, whom for confidentiality’s sake I will call Dr. Hermes. An anesthesiologist in his early sixties and now retired, he was a physician who often served on obstetric cases at Baptist Hospital in Jacksonville.
During the session, the conversation turned to August’s birth, and, at his behest, she told him the story. When she finished, he remained silent for a moment, and then he said, “I can’t say for certain what happened. But this sounds like a classic case of an obstructed labor.” He went on to explain: “This is also known as labor dystocia, and it occurs because the baby can’t exit the pelvis during childbirth due to being blocked. This happens even if the uterus is contracting normally.”
“I had a lot of pain in my pelvic area despite the epidural,” Ilene said.
“His head might have been hitting against the pelvic bone,” Dr. Hermes went on. “It’d be like ramming your head into a door, slowly but repeatedly. Like this,” he said, and he slammed his fist into his palm, then paused, then slammed it again, and again paused. Bam! Pause. Bam! Pause. Bam! Pause. Bam!
Stories of medical errors are easy to dismiss, but a close family member of his had recently experienced a serious one, so he was open to the idea. And then he said something that was unprecedented, for us at least: “Someone should have noticed,” he told Ilene, “that the labor wasn’t progressing and ordered a C-section. I am truly sorry that August received such poor care. That shouldn’t have happened.”
“Then a medical error isn’t just a figment of our imaginations?”
He chuckled quietly, shook his head, and said, “Is that what they wanted you to believe? Listen, here’s what probably happened. It’s not complicated. August experienced fetal distress during the delivery, and maybe he was experiencing it in the days leading up to the delivery. But whenever it started, it wasn’t detected, and as a result he suffered severe brain injury and cerebral palsy. And that’s why he had the life he did.”
For sixteen years we had sought to solve the riddle of what had happened in the V.I.P. birth suite. What happened to our son? What accounted for the “never event”? No physician had ever been willing to offer an explanation. But Dr. Hermes was willing to venture an educated guess. And now, two years after August’s death, we had an answer to the riddle of his birth. The answer to a riddle always seems so obvious once it is revealed.